- Volume 60 , Number 3
- Page: 466–9
Hansen, 150 years after his birth, the context of a medical discovery
Why do we celebrate?
Gerhard Henrik Armauer Hansen, the discoverer of the leprosy bacillus, was born in Bergen, Norway, on 29 July 1841. In 1991, 150 years later, during a commemorative seminar, one may ask why we are celebrating. At least three different reasons, all important, seem obvious.
First of all, a heritage is being celebrated. The memory of Gerhard Henrik Armauer Hansen is certainly not only a family heritage, it is not even only a heritage of a city or a nation. We are celebrating an international heritage of strong, professional, scientific significance rooted in the initiation of leprosy Research, but also with an important bearing on the international community at large, linked with humanitarian values. The heritage evokes humble gratitude to Hansen's efforts and achievements for the benefit of following generations. Thus, the heritage involves a celebration in retrospect to express thanks and appreciation.
Secondly, aspects are involved today which concern ourselves. Hansen set an example that might inspire and create enthusiasm even today. For his countrymen, belonging to a small nation and perhaps feeling a bit timid in an international context, this example might be linked with positive elements of national pride as well. We often feel that Hansen put the name of Norway on the medical map of the world. Thus, Hansen paved a path for subsequent candid and not so candid countrymen, a path many of us have seen and some of us have walked over the years, a path which seems .more distinctive the further you travel from Norway.
Finally, and in my mind the most important aspect of the celebration: the implications that point ahead into the future. By paying homage to past achievements, we give important signals to following generations. This relates to the way we esteem science and the scientist in our community and, thus, to future recruitment. Homage to outstanding predecessors in science conveys to the youth of today that the community treasures science as well as the scientist. Thereby, science may recruit the best, also in the future, and the basis for scientific progress is secured.
Consequently, we have a series of good reasons to celebrate today. However, after having recently read Hansen's memoirs1 once again, I feci quite confident that he, in his partially self-cynical way, would have stressed this third reason for celebrating. Being a dedicated and devoted nonreligious man, he might have added in his memoirs that the celebration should not and would not have contributed any personal benefits to himself, at the moment.
On occasions like the present, there is always a duty to be performed. I am entrusted with the privilege of taking you through the duties, which I will try to address in this third perspective, a perspective raising a few questions.
Motivation
Why did Hansen choose leprosy? Why were physicians in Hansen's time challenged by this disease? In general, and now aiming at future recruitment, are there any motives for embarking on a fight against a serious public health problem, motives other than those always involved related to personal prestige and career? How about feelings such as responsibility, solidarity, moral duty?
This country still has a lot of unspoiled and untouched nature which impresses its inhabitants, nature which was only discovered by the urban population during the last century. A series of talented contemporary painters displayed their almost religious relationship with this nature. Ibsen wrote his "Brand," a dramatic poem concentrating on Peer Gynt's counterpart, the clergy and his burden of duties; in a double way staged against the marvellous, but also overwhelming nature of Norway.
However, this nature also had its inhabitants. Thus, an increasing awareness toward the rural population and its problems evolved. This interest focused not only on nationalistic, romantic aspects. Illustrations of serious medical problems, i.e., leprosy, existed as long ago as the beginning of the last century, depicting several of the 150 inmates of St. George's Hospital in Bergen around 1815.2 These primitive drawings were intended to awaken the conscience of the contemporary medical authorities to the Norwegian leprosy problem and represented the initiation of the great crusade against leprosy in Norway which lasted throughout the 19th century.
What was the magnitude of the leprosy problem at that time? In the two West coast counties around Bergen alone there were altogether 1500 patients or 5 per 1000 inhabitants while 5 per 10,000 died from leprosy each year.3 This amounted to more than 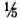 of the mortality of the great "killer," tuberculosis, toward the end of the same century. With a considerably longer duration of the disease, leprosy must have represented a comparably larger problem.
of the mortality of the great "killer," tuberculosis, toward the end of the same century. With a considerably longer duration of the disease, leprosy must have represented a comparably larger problem.
Initiation
Obviously these figures were not known at the time, but there was an increasing feeling that the situation should be assessed and appropriate measures taken.2 Thus, in 1832, J. J. Hjort (1798-1873) traveled around the districts in western Norway to study skin diseases, and was instructed by the central health authorities to pay special attention to leprosy. His conclusions were that the leprosy sufferers had terrible living conditions, that their needs for care and nursing were not sufficiently met-and perhaps a bit surprisingly-that leprosy was curable. This report seemed to arouse the central health authorities who approached the problem from three different angles.
From a pathology perspective, D. C. Danielssen (1815-1894) established the disease as a nosological entity based on scientific criteria developed after meticulously performed autopsy examinations.4
This led to an impressive achievement from a clinical perspective: first the foundation in 1849 of a leprosy Research hospital for 90 patients, and subsequently the erection, during the following years through 1861, of an additional three hospitals with more than 1000 beds for leprosy patients only. The total number of patients in Norway at any one time never exceeded 2700.
Uncertainty as to the magnitude of the leprosy problem led to activities which were important from an epidemiological perspective. Leprosy censuses were conducted in 1836, 1845, and 1852 and they reported increasing numbers of patients, as well as enormous methodological problems related to the ascertainment of cases.3 Consequently, a Royal Decree of 1856 authorized the foundation of the National Leprosy Registry of Norway,5 as well as the establishment of local Boards of Health consisting of members of the municipality council appointed to assist the District Health Officer in case finding and in other local preventive activities. The first Chief Medical Officer for Leprosy in Norway, O. G. Hoegh (1814-1863) attached great importance to the Leprosy Registry. It was on the basis of these data, he asserted, that the clue to the cause of the disease would be found. Already in 1858 he claimed that the data accumulated so far gave support to the hypothesis that leprosy was an infectious disease.
Contemporary scenario
Gerhard Hcnrik Armauer Hansen was born 29 July 1841, the year after Danielssen was asked by the Norwegian Parliament to continue his scientific Research, and the year before the decision was made to establish Lungegaards Hospital, the Research hospital. Hansen was the family name, while the more uncommon Armauer originated from the maternal grandmother; her brother was Gerhard Henrik Armauer, a carpenter of high local reputation.
In 1866, Hansen graduated from medical school in Oslo, and after a few years, started his work in the three leprosy hospitals in Bergen and, in particular, the Research hospital. The contemporary European epidemiological context comprised the well-established general concept of infectious etiology.6 Around 1850, J. Snow (1813- 1858) had published his work on the spreading of cholera through contaminated drinking water, and in 1861, I. Semmelwciss (1818-1865) had published his observations on the infectious character of puerperal fever. From a theoretical point of view, the concept emerged through principles already formulated in 1840 by J. Henle (1809- 1885), addressing the way to prove a causeeffect relationship between a microorganism and a disease. The first microorganism to be described according to these principles was Bacillus anthracis, discovered in 1869 by C. Davaine (1812-1882).
All this was well known in contemporary Norway where similar scientific contributions were made.6 Between 1859 and 1865, C. Homan( 1826-1880) and C. H. Hartwig (1824-1892) conducted field studies on dysentery and typhoid, inferring the existence of infectious agents responsible for the propagation of these diseases. In 1869, E. F. G. Winge (1827-1897) and H. Heiberg (1837-1897) described rosary-like threads on heart valves in a patient who had died of septicemia.
Hansen was definitely aware of all this information, and soon he entered the vivid discussion of the etiology of leprosy. The majority, headed by Danielssen (now Hansen's father-in-law) claimed that leprosy was a hereditary disease. Another group "maintained that leprosy was an unspecific degeneration caused by harsh living conditions. Finally, a third group was convinced that leprosy was an infectious disease. Hansen belonged to the last group, and found evidence to support the view in his treatise of 1874 7in which he pointed out that the disease had decreased much faster in areas where hospitalization had been enforced most consistently; here, the chain of infection had been most effectively intermitted. Toward the end of his treatise, he accounted for what he considered to be his discovery of the infective agent of leprosy. His first successful attempt to make this agent visible is carefully described with the date and even the name of the patient from whom the material was taken. There are moments in the history of medicine that should never be forgotten. One of those is 28 February 1873.
Struggle for proof and priority
This discovery led to two, perhaps unexpected, chapters in Hansen's life. However, there were other important events which were to take place before that. Later the same year, Hansen's wife died of tuberculosis. In 1875, Hansen was appointed Chief Medical Officer for Leprosy. In 1877, Hansen had his first law against leprosy adopted by the Parliament, "Act for the maintenance of poor leprosy patients," by which the old system of boarding out was prohibited for leprosy sufferers.
But then in 1879, Hansen was visited in Bergen by A. Neisser (1855-1916) who, in 1880, claimed that he himself had discovered the leprosy bacillus. Neisser argued on the basis of the fact that he had succeeded in staining the bacillus. The same year, Hansen wrote a paper in German about which he ascertained in his memoirs that "this paper effectively established the fact that it was I who found the cause of leprosy."1 From this fight for priority rose a nationalistic storm of support among colleagues in Norway, a support that would prove of great value to Hansen later the same year.
Hansen was aware of Henle's principles, viz., that the microorganism should 1) be present in all patients with the disease, 2) be cultivable outside the human or animal organism, and 3) induce a disease similar to that in man upon inoculation into an animal. Thus, Hansen made altogether 12 attempts, all in vain, to inoculate the bacillus into rabbits and volunteers including himself. Then, he inoculated leprous tissue from a patient with lepromatous leprosy into the eye of a patient with tuberculoid leprosy. For that reason, Hansen was "charged with undertaking, without the patient's consent and against her wishes, an operation which apparently had not caused, and possibly could not cause, lasting damage to her eye, but had nevertheless occasioned her much anxiety and not inconsiderable pain."8 On this basis, Hansen was sentenced to forfeiture of his post as physician at the hospital where the experiment had been undertaken, but he retained the position as Chief Medical Officer for Leprosy.
In 1885, the second law, "Act on the seclusion of leprosy patients," was passed. The law prescribed isolation of the patients, either in a separate room in their homes or, if this was not possible, in one of the leprosy hospitals.
Final recognition
All these breathtaking events occurred during a period of less than 15 years. Eventually, the Norwegian model for dealing with the leprosy problem won international recognition. In 1897, at the First International Leprosy Congress in Berlin, the following resolution was adopted: "The system of compulsory notification, surveillance and isolation of patients, as implemented in Norway, should be recommended in all countries with autonomous municipalities and a sufficient number of physicians."2 No doubt, this attitude of the international scientific community also must have represented enormous support and recognition for Hansen. This attitude was expressed at the celebration of Hansen's 60th birthday in 1901, and at the Second International Leprosy Congress in Bergen (1909) where Hansen was the president.
Surprisingly, the recognition of leprosy as an infectious disease developed in spite of the fact that Henle's three principles were not fulfilled until more than half a century after Hansen's death in 1912. Problems related to the cultivation of Mycobacterium leprae and the development of animal models were not the only obstacles to the correct understanding of the nature of this disease. With a long-range incubation period, in some cases up to 20 years, epidemiologic inference in leprosy as to causation is extremely complicated. We may certainly be impressed by the way our colleagues in the last century arrived at a correct conclusion of infection. From a practical point of view, the establishment of leprosy as an infectious disease and its inherent consequences in terms of public health measures was the significant implication of Hansen's discovery. This was, perhaps, Hansen's greatest contribution to the fight against leprosy.
- Prof. Lorentz M. Irgens, M.D.
Section of Preventive Medicine
Institute of Community Medicine
University of Bergen
Haukeland Hospital
N-5021 Bergen, Norway
1. Hansen, G. H. A. The memories and reflections of Dr. Gerhard Armauer Hansen. Wurzburg, 1976.
2. Irgens, L. M. Leprosy in Norway: an interplay of Research and public health work. Int. J. Lepr. 41(1973)189-198.
3. Irgens, L. M. Leprosy in Norway; an epidemiological study based on a national patient registry. Lepr. Rev. 51 Suppl. 1(1980)1-130.
4. Danielsen, D. C. and Boeck, C. W. Traite de la Spedalskhed ou Elephanthiasis des Grees. Paris, 1848.
5. Irgens, L. M. and Bjerkedal, T. Epidemiology of leprosy in Norway: the history of the National Leprosy Registry of Norway from 1856 until today. Int. J. Epidemiol. 2(1973) 81-89.
6. Irgens, L. M. The discovery of Mycobacterium leprae; a medical achievement in the light of evolving scientific methods. Am. J. Dermatopathol. 6(1984)337-343.
7. Hansen, G. H. A. Undersogelser angaaende Spedalskhedens Aarsager. Norsk Mag. f. Laegev. 4 Suppl.(1874)1-88.
8. Blom, K. Armauer Hansen and human leprosy transmission; medical ethics and legal rights. Int. J. Lepr. 41(1973)199-207.