- Volume 69 , Number 2
- Page: 130–74
Current literature
This department carries selected abstracts of articles published in current medical journals dealing with leprosy and other mycobacterial diseases.
GENERAL AND HISTORICAL
Diletto, C. and Blanc, L. Leprosy chemoprophylaxis in Micronesia. Lepr. Rev. 71 Suppl.(2000)S2I-S25.
A program of chemoprophylaxis was introduced as a component of the leprosy control program in the Federated States of Micronesia (FSM), beginning in 1996. The entire population of the country was to be screened, and a single dose of 600 mg rifampin, 400 mg ofloxacin and 100 mg minocycline (ROM) was to be administered to the entire population. Two rounds of screening the entire population were carried out, approximately 1 year apart, and chemoprophylaxis was administered at the time of each screening. Ninety percent of the population were screened at least once, and 55% were screened in both rounds; 87% of the populations received at least one dose, and 54% received two doses. In the course of the first round, 322 new cases were detected; whereas only 80 new cases were detected during the second round, of whom only 12 had received chemoprophylaxis in the course of the first round. A third round of screening, confined to a small number of villages in both Chuuk and Pohnpei, in which states leprosy endemicity was high, was carried out approximately 2 years after the second. Only 16 new cases were detected during the third round of screening; whereas 102 new cases had been detected in this same population during the first round of screening, and 32 new cases during the second. Six of the 16 newly detected cases stated that they had been administered chemoprophylaxis at least once; however, this information may not be reliable.-Authors' Summary
Ginsberg, A. M. Leprosy research-setting priorities and facilitating collaborations: a personal perspective. Lepr. Rev. 71 Suppl.(2000)S183-S187.
In recent years, as the prevalence of leprosy has declined and the tuberculosis epidemic has gained increasing attention, leprosy research has generally taken a "back seat" to research in tuberculosis and other emerging and re-emerging infections. This has resulted as much from perceived differences of scientific opportunities in these fields as from differences of the disease burden. At the United States National Institutes of Health (NIH), research priority setting is typically based on a number of factors. In the case of leprosy research, the technical difficulties associated with this scientific area have clearly lessened enthusiasm for and progress in this field. Today, however, we are confronted by the reality of not having sufficient scientific understanding to explain a stable or increasing number of leprosy cases detected annually in the face of a dramatically decreasing total number of identified cases. We also lack adequate tools for diagnosis and prevention. At the same time, new molecular and cellular approaches and knowledge of the complete sequence of the genome of Mycobacterium leprae render leprosy research significantly more tractable than ever before. The combination of these factors has led a number of groups, including the National Institute of Allergy and Infectious Diseases of the NIH, to review the current state of knowledge in leprosy research and draft recommendations for future leprosy research priorities. It is clear that many of the necessary and exciting research activities can best be addressed through collaborations among investigators, with control programs, and among countries of high and low endemicity.-Author's Summary
MILEP2 Study Group. Approaches to studying the transmission of Mycobacterium leprae. Lepr. Rev. 71 Suppl.(2000)S26-S29.
A collaborative study has been undertaken to establish the relationship between infection by Mycobacterium leprae and the development of immunity in a community in which multidrug therapy (MDT) has been used for more than 10 years, to elucidate the pathogenesis of infection in leprosy, and to develop and test an intervention strategy based on chemotherapy for interruption of transmission of the organism in the community. The first phase of the study included the establishment of laboratory facilities and pilot work in India. In the course of the second phase, the entire populations of three villages in India and one in Ethiopia have been surveyed, nasal swabs were obtained for detection of M. leprae DNA by means of the polymerase chain reaction (PCR), specimens of saliva were obtained for measurements of levels of antiM. leprae IgA antibodies, and follow-up surveys have been carried out. A doubleblind trial of chemotherapy among subjects whose PCR was positive is proposed to determine if the course of the infection can be influenced by treatment. The performance of large numbers of PCR tests in endemic countries has required the development of rigorous internal and external quality control procedures. These have shown that many batches (as many as 50%) fail to meet quality control criteria, and must be retested. Despite this, development of these methods and their application to field studies should provide tools for studying the transmission of M. leprae, and direct methods of testing innovative interventions.Authors' Summary
Nguyen, L. N., Cartel, J. L. and Grosset, J. H. Chemoprophylaxis of leprosy in the Southern Marquesas with a single 25 mg/kg dose of rifampicin. Results after 10 years. Lepr. Rev. 71 Suppl.(2000)S33-S36.
In 1988, a program of leprosy chemoprophylaxis, employing a supervised, single 25 mg/kg dose of rifampin, was implemented in the Southern Marquesas Islands. Of the 2786 inhabitants, 2751 (98.7%) were treated. In addition, 3144 South Marquesans living elsewhere in French Polynesia were administered the same chemoprophylaxis. During the following 10 years, seven leprosy patients were detected among those who had been administered chemoprophylaxis. Of these, two were very likely missed cases of leprosy, and cannot be considered a failure of chemoprophylaxis. The epidemiometric projection model, based on cases of leprosy observed in the Southern Marquesas during the 20 years preceding implementation of the program, predicted that 17 leprosy cases could be expected in the South Marquesan population if no chemoprophylaxis were given. In fact, only five cases were detected in the treated population, a number significantly smaller than 17, suggesting that the chemoprophylaxis was 70% effective, assuming that no change of detection rate would have occurred without chemoprophylaxis. However, during the 10 years following implementation of the chemoprophylaxis program, the detection rate in the Polynesian population that was not administered chemoprophylaxis declined by about 50%. Therefore, the effectiveness of the chemoprophylaxis was only 35%-40%.-Authors' Summary
Nordeen, S. K. Leprosy research and elimination. Lepr. Rev. 71 Suppl.(2000)S12-S14.
The contribution of leprosy research to the progress being made toward elimination of leprosy has been critical. A major development in the promotion of leprosy research during the last 25 years has been the initiative taken by the WHO Special Programme for Research and Training in Tropical Diseases (TDR) through two of its scientific working groups, one on the immunology of leprosy (IMMLEP) and the other on the chemotherapy of leprosy (THELEP), which were set up in 1974 and 1976, respectively. IMMLEP and THELEP have greatly facilitated input from scientists not usually active in leprosy research. The coordinated efforts of IMMLEP and THELEP also facilitated goal-oriented research toward high-priority target areas such as an antileprosy vaccine and newer and better drug-combinations for the treatment of leprosy. Whereas the prospects for a leprosy vaccine appeared very promising in the yearly years, the first vaccine produced did not meet expectations for several reasons. Moreover, the possibility of using a vaccine in leprosy is not bright, because of both the technical problems as well as the reduced relevance of a vaccine at a time when leprosy is becoming less and less common. On the other hand, the modest expectations for newer and better drug combinations led to multidrug therapy (MDT) for the control of leprosy. It is the introduction of MDT that is credited with the current global reduction of leprosy and the progress thus far made toward eliminating the disease as a public health problem. Nevertheless, many areas in leprosy, such as nerve damage, remain that require major research input in the future.-Author's Summary
Nordeen, S. K. Prophylaxis-scope and limitations. Lepr. Rev. 71 Suppl.(2000)S16-S20.
Attempts to prevent leprosy by one or another prophylactic method began with the use of dapsone as a chemoprophylaxis. Following early, small-scale studies, which were promising, large-scale studies with dapsone and acedapsone, both among contacts and in the general population, demonstrated that it is possible to prevent the occurrence of leprosy to a modest extent. With regard to immunoprophylaxis, BCG had long been considered a possibility, particularly in view of its potential to convert the skin test reaction to lepromin. Over the years, major, large-scale field trials of BCG had been carried out in Uganda, Burma, Papua New Guinea and India. All of the studies demonstrated that BCG was capable of preventing leprosy. However, protective efficacy varied from around 20% to greater than 80%. Killed Mycobacterium leprae mixed with BCG has also given varying results. Other vaccines based on cultivable mycobacteria have also been tried, and at least one of them appears promising. An approach to prophylaxis must taken into account a) the level of risk addressed and the perception of risk by the community; b) the level of efficacy of the method of prophylaxis; c) the possibility of easily identifying high-risk groups; d) the operational feasibility; and e) the focus of the prophylaxis, whether the individual or the community, or both. However, in view of the enormous progress being made toward elimination of leprosy by the widespread application of MDT, prophylaxis is becoming less and less relevant and less and less cost-effective, except in very special situations.-Author's Summary
Obregon, D. [Leprosy and bacteriological research in Colombia: studies of Carrasquilla and Lleras.| Biomédica 20(2000)181-189. (in Spanish)
The history of leprosy research in Colombia is discussed, including clinical and bacteriological studies.-Trop. Dis. Bull. 98(2001)941
Ooi, W. W. and Moschella, S. L. Update on leprosy in immigrants in the United States: status in the year 2000. Clin. Infect. Dis. 32(2001)930-937.
The World Health Organization established a goal in 1991 of "elimination of leprosy as a public health problem by the year 2000." Although prevalence rates of leprosy have decreased in many geographic areas, it is clear that in some countries where leprosy is endcmic, such as Brazil and India, this goal will not be reached. Leprosy is rare in the United States, but 85% of detected cases are immigrants in whom the disease may mimic many common dermatologie and neurological entities, leading to delay of diagnosis. The statuses of polymerase chain reaction analysis, serological testing, and vaccines are reviewed. Effective multidrug therapy and prevention of permanent damage to nerves by early recognition and treatment will help prevent residual disabilities. This update reviews what is known about the pathophysiology and treatment of leprosy. Increased awareness will lead to earlier recognition, diagnosis, and treatment.-Authors' Abstract
Pinto Neto, J. M., Villa, T. C. S., do Oliveira, M. H. P. and Barbeira, C. B. S. [The control of leprosy contacts in Brazil: a review.] Hansen. Int. 25(2000)163-176. (in Portuguese)
This work is a synopsis of a literature review about the control of leprosy contacts in Brazil according the three periods from the year of Republic Proclamation up to today. Along this review we try to rescue the chronology of facts which concern leprosy, contacts, control, emphasizing scientific publications, the laws on it, and directives about the program of leprosy control at state and national levels.-Authors' English Summary
Rao, P. V. R., Bhuskade, R. A. and Desikan, K. V. Modified leprosy elimination campaign (MLEC) for case detection in a remote tribal area in the State of Orissa, India. Lepr. Rev. 71(2000)377-381.
A leprosy project was established in a difficult-to-reach area under guidelines of the government of India. The leprosy services were provided by Koraput Leprosy Eradication Project (KORALEP) and general health services by Primary Health Care (PHC). Leprosy elimination campaigns (LECs) were suggested by WHO to detect more cases in the community. A modified leprosy elimination campaign (MLEC) carried out utilizing the services of primary health care workers is discussed in this paper. Apart from the trained health workers, Anganwadi workers along with some literate people from the district were also included in the search teams. In all, 1543 cases were shortlisted from the suspects identified and on re-examination 576 cases were confirmed as active cases. Sixty percent of the cases detected were very early cases with two to three skin lesions. This could be achieved with a very brief training of health workers and involving village voluntary workers. MLEC was found to be a useful tool for case finding in such areas.- Trop. Dis. Bull. 98 (2001) 1679
Rojas-Espinosa, O. and Lovik, M. Mycobacterium leprae and Mycobacterium leprae/milium infections in domestic and wild animals. Rev. Sci. Tech. 20(2001)219-251.
Mycobacterium leprae, the etiological agent of leprosy in humans, gives rise to a chronic granulomatous disease that affects primarily the skin and peripheral nerves and, secondarily, some internal organs such as the testis and the eye; viscera are seldom involved. Depending on host resistance, leprosy may present as a benign disease (tuberculoid leprosy) or as a malignant disease (lepromatous leprosy), with a spectrum of intermediate stages appearing between the two. Immunity against leprosy depends on the cell-mediated immunity of the host, and this is severely compromised in the malignant (lepromatous) form of leprosy. Although culture of M. leprae has never been achieved in artificial media, the bacterium may be grown in several experimental animals, including the armadillo, nonhuman primates and, to a certain extent, rodents. Naturally acquired leprosy has been reported in wild nine-banded armadillos (Dasypus novemcinctus) and in three species of nonhuman primates [chimpanzees (Pan troglodytes), sooty mangabey monkeys (Cercocebus atys) and cynomolgus macaques (Macaca fascicularis)], thus qualifying leprosy as a zoonosis. Murine leprosy is a leprosy-like disease of rats and mice caused by M. lepraemurium. The disease affects primarily viscera and the skin, and very rarely peripheral nerves. Depending on the host strain, rodent leprosy may also evolve as "lepromatous" or "tuberculoid" leprosy, and strains of mice that develop intermediate forms of the disease may exist. Growth of M. lepraemurium on conventional media for mycobacteria is not successful, but the bacterium has been cultured on an egg yolk-based medium. Naturally acquired murine leprosy has been observed in rats, mice and cats but not in humans or any other species. Thus, in contrast to human leprosy, murine leprosy is not a zoonosis.-Authors' Abstract
Sabroza, P. C., dos Santos, E. M., Andrade, V. and Hartz, Z. (Operational research in leprosy public health surveil lance-a proposal.] Hansen. Int. 25(2000)143-146. (in Portuguese)
Communicable diseases such as leprosy remain a preventable factor to the social and economic development of Brazil. In this country the National Council of Municipal Health Secretaries has introduced a task force to accelerate the elimination of leprosy with the purpose of helping local managers to accomplish the mission of providing full access of communities to health services capable of diagnosing, treating and curing leprosy cases. However, the transition period for different proposals of controlling endemic diseases shows some constraints due to complex factors not well known. In this regard, a better understanding of how behavior, political attitude and the allocation of financial resources to the health sector are factors that act and modify the patterns of this disease is of utmost importance to orient efforts toward its elimination. Without eliminating traditional activities, the main ax of this new approach would be the decisions regarding the perspective of promotion and protection of health in an ample way in order to integrate these activities in the health care .issues avoiding the disciplinary and bureaucratic fragmentation present in its way of acting. This ax is coincident, in part, to some research lines recently proposed by WHO. In this regard, the authors suggest four axes for operational research in the field of leprosy in Brazil: the integrality of care, the quality of care, sustainability and regulation. They also present some details of components of the four axes aiming to contribute to an ample national and international discussion in this field of operational research.-Authors' English Abstract
Shah, G., Pai, V. V., Revankar, C. R. and Ganapati, R. "Wall Journal" on leprosy-a novel method to educate medical students. Lepr. Rev. 71(2000)388-389.
Undergraduate medical students (N = 50) and postgraduates and faculty (N = 30) in four medical colleges in India were asked to answer a questionnaire to determine the impact of the "Wall Journal" (WJ; updated information on leprosy put on display in the medical colleges every month starting July 1991) dissemination of information on leprosy: 80%-90% of the respondents found that the WJ was useful in their academic research work and in preparing for the leprosy competitive examination; 60%-70% felt the need for more pictures and clinically oriented material; 20% thought that the contents of the WJ should be comprehensive enough to enable them to read the material displayed in the shortest possible time; 90% of respondents noted that the WJ should be posted at the central and most frequented places; 10% thought that there is a need to improve the quality of the WJ in order to make it more attractive. All of the respondents emphasized the need to continue the WJ which has become one of the most important sources of information on leprosy.'Trop. Dis. Bull. 98(2001)1660
Vijayakumaran, P., Krishnamurthy, P., Rao, P. and Declerq, E. Chemoprophylaxis against leprosy: expectations and methodology of a trial. Lepr. Rev. 71 Suppl.(2000)S37-S41.
Because of the great efficacy of multidrug therapy (MDT), it had been hoped that the widespread use of MDT would bring about a rapid decrease of the incidence of leprosy. To the present, a decrease of incidence has not been observed, possibly because of the long incubation period of the disease, and because general implementation of MDT is still recent. Other reasons, such as environmental sources of infection or the role of healthy carriers in transmitting Mycobacterium leprae, cannot be excluded. Therefore, one must seek alternative or supplementary strategies, such as chemoprophylaxis. Household contacts of leprosy patients are at greater risk of developing leprosy than is the general population. Therefore, a randomized, controlled trial of chemoprophylaxis, using a single 10 mg/kg dose of rifampin, or a placebo, is planned in nine projects in India among the household contacts of newly detected leprosy patients. Based upon assumptions of a protective efficacy of the chemoprophylaxis of 50%, an annual incidence of 2 per 1000 contacts, a desired power of the study of 90%, and a level of significance of 95%, 15,000 household contacts will be allocated randomly by household to each arm of the study, and followed for 5 years. Considered as household contacts will be all persons living in the same household as an index case and sharing the same kitchen. Pregnant women and infants will be excluded. To be certain that transmission of the organisms from the index case cannot occur once the prophylaxis is administered, rifampin will be administered 2 months after diagnosis of the index case. Diagnosis of leprosy will be clinical, and confirmed independently. Although household contacts usually constitute only a small proportion of the new patients detected in a control program, their high-risk status makes them particularly appropriate for a study of the potential effect of chemoprophylaxis. Following the trial, one could evaluate the usefulness and feasibility of using the same strategy in other population groups, based on the number of persons necessary to treat to prevent one case.-Authors' Summary
Whitcher, J. P., Srinivasan, M. and Upadhyay, M. P. Corneal blindness: a global perspective. Bull. WHO 79(2001)214-221.
Diseases affecting the cornea are a major cause of blindness worldwide, second only to cataract in overall importance. The epidemiology of corneal blindness is complicated and encompasses a wide variety of infectious and inflammatory eye diseases that cause corneal scarring, which ultimately leads to functional blindness. In addition, the prevalence of corneal disease varies from country to country and even from one population to another. While cataract is responsible for nearly 20 million of the 45 million blind people in the world, the next major cause is trachoma which blinds 4.9 million individuals, mainly as a result of corneal scarring and vascularization. Ocular trauma and corneal ulceration are significant causes of corneal blindness that are often underreported but may be responsible for 1.5-2.0 million new cases of monocular blindness every year. Causes of childhood blindness (about 1.5 million worldwide with 5 million visually disabled) include xerophthalmia (350,000 cases annually), ophthalmia neonatorum, and less frequently seen ocular diseases such as herpes simplex virus infections and vernal keratoconjunctivitis. Even though the control of onchocerciasis and leprosy are public health success stories, these diseases are still significant causes of blindness-affecting a quarter of a million individuals each. Traditional eye medicines have also been implicated as a major risk factor in the current epidemic of corneal ulceration in developing countries. Because of the difficulty of treating corneal blindness once it has occurred, public health prevention programs are the most cost-effective means of decreasing the global burden of corneal blindness.-Authors' Abstract
CHEMOTHERAPY
Attri, S., Rana, S. V., Vaiphei, K., Sodhi, C. P., Katyal, R., Goel, R. C., Nain, C. K. and Singh, K. Isoniazidand rifampicin-induced oxidative hepatic injury-protection by N-acetylcysteine. Hum. Exp. Toxicol. 19(2000)517-522.
The role of N-acetylcysteine (NAC), a glutathione (GSH) precursor, was investigated in protection against isoniazid (1NH)and rifampin (RlF)-induced oxidative hepatic injury in young Wistar rats. The hepatoxic dose of INH and RIF was 50 mg kg-1 day-1 each and the hepatoprotective dose of NAC was 100 mg kg-1 day1. All drugs were administered intraperitoneally (i.p.) in sterile water [4.0 ml k-1 day-1) over a period of 3 weeks. Status of oxidative/antioxidative profiles was the mechanistic approach to assess the hepatotoxicity and/or hepatoprotection. The oxidative injury in INH-RIF co-exposed animals was closely associated with significant decline of GSH and related thiols, as well as with compromised antioxidant enzyme system. The oxidative stress was further supported by increased lipid peroxidation observed in these animals. The co-administration of NAC prevented the induction of oxidative stress in INH-RIF coexposed animals. The amelioration of oxidative stress by NAC was faithfully reflected as normal morphology in these animals, except the presence of mild degree of portal triaditis in one animal co-exposed to INH-RIF and NAG. In contrast, the animals co-exposed to INH-RIF alone showed histological lesions which ranged from intralobular inflammation to patchy necrosis. These results suggest that INH-RIF-induced oxidative injury can be prevented by supporting the cellular antioxidant defense mechanism by NAG.-Authors' Abstract
Campbell, E. A., Korzheva, N., Mustaev, A., Murakami, K., Nair, S., Goldfarb, A. and Darst, S. A. Structural mechanism for rifampicin inhibition of bacterial RNA polymerase. Cell 104(2001)901-912.
Rifampin (Rif) is one of the most potent and broad spectrum antibiotics against bacterial pathogens and is a key component of anti-tuberculosis therapy, stemming from its inhibition of the bacterial RNA polymerase (RNAP). We determined the crystal structure of Thermus aquaticus core RNAP complexed with Rif. The inhibitor binds in a pocket of the RNAP beta subunit deep within the DNA/RNA channel, but more than 12 A away from the active site. The structure, combined with biochemical results, explains the effects of Rif on RNAP function and indicates that the inhibitor acts by directly blocking the path of the elongating RNA when the transcript becomes 2 to 3 nt in length.-Authors' Abstract
Grosset, J. The new challenges for chemotherapy research. Lepr. Rev. 71 Suppl.(2000)S100-S104.
Scientific knowledge is constantly expanding, and needs are changing; therefore, efforts must be made to adapt the treatment of leprosy and the manner in which it is implemented to the newly identified needs. Because an effective vaccine against leprosy remains to be identified, multidrug therapy (MDT) is the only tool available for leprosy control. At present, therefore, the priority is to make MDT available in all endemic countries for all patients, even those living in difficult-to-access areas. The remaining important issues in chemotherapy research are to improve the quality of leprosy case finding, improve the quality of MDT, identify the areas in which leprosy patients are not receiving proper MDT, and find the means necessary to ensure delivery to all of appropriate MDT. The MDT regimens recommended by the World Health Organization are of too long duration, require correct classification of the patients as PB or MB, and rely upon the daily self-administration of dapsone and clofazimine to prevent selection of rifampin-resistant mutants among MB patients. Thus, research leading to the development of new drug regimens should be directed toward overcoming the shortcomings of the presently recommended regimens. The drugs required to permit use of regimens of shorter duration, that may be employed among both PB and MB patients, and that enable fully supervised drug administration may be already in hand, and the necessary clinical trials to confirm efficacy and acceptability should be carried out.-Author's Summary
Ji, B. Prospects for chemotherapy of leprosy. Indian J. Lepr. 72(2000)187-198.
A review of standard and new generation multiple drug therapy regimens for the treatment of Mycobacterium leprae infection is presented. The development of new generation MDT regimens with powerful bactericidal activity against M. leprae is discussed. Available new antileprosy drugs and two new generation MDT regimens are described.-Trop. Dis. Bull. 98(2001)924
Ji, B. and Grosset, J. Combination of rifapentine-moxifloxacin-minocycline (PMM) for the treatment of leprosy. Lepr. Rev. 71 Suppl.(2000)S81-S87.
To further the development of a multidrug regimen for treatment of leprosy that is suitable for monthly administration and fully supervisable, the bactericidal activities against Mycobacterium leprae of HMR 3647 (HMR), moxifloxacin (MXFX) and rifapentine (RPT) were measured by the proportional bactericide technique in the mouse foot pad system, and compared with those of the established antileprosy drugs clarithromycin (CLARI), ofloxacin (OFLO) and rifampin (RMP). Administered in five daily doses of 100 mg per kg body weight, HMR appeared slightly more bactericidal than CLARI, but the difference did not attain statistical significance. Administered as single doses, MXFX in a dosage of 150 mg per kg was more active than OFLO in the same dosage, and displayed the same level of activity as RMP in a dosage of 10 mg per kg; the combination MXFXminocycline (MINO) (MM) was more bactericidal than the combination OFLOMINO (OM); RPT in a dosage of 10 mg per kg was more bactericidal than RMP administered in the same dosage, and even more active than the combination RMP-OFLOMINO (ROM); the combination RPTMXFX-MINO (PMM) killed 99.9% of viable M. leprae, and was slightly more bactericidal than was RPT alone, indicating that the combination PMM showed an additive effect against M. leprae. These promising results justify a clinical trial among lepromatous patients, in which MM is being compared with OM, and PMM with ROM, in terms of efficacy and tolerance.-Authors' Summary
Li, H. Y., Ran, S. P., Weng, X.-M., Li, T.G., Deng, X.-H. and Li, F. T. Relapses in leprosy patients treated with rifampicin plus dapsone after varying periods of dapsone monotherapy. Indian J. Lepr. 73(2001)1-10.
Leprosy patients treated formerly with dapsone monotherapy followed by combined therapy with rifampin plus dapsone were surveyed for relapse and rifampin resistance. The relapse rate was significantly low for the 482 multibacillary (MB) patients receiving >12 months combined therapy compared with the 49 MB cases receiving <12 months of combined therapy. The relapse rate was related to the duration of dapsone monotherapy prior to combined therapy. The difference in relapse rate in 247 paucibacillary (PB) patients following >12 months combined therapy was also of significance, compared with the 66 PB cases who had received <12 months combined therapy. Five strains of M. leprae isolated from relapsed patients were sensitive to rifampin by mouse foot pad test and all relapsed patients responded favorably to fixed duration MDT regimen for MB cases.-Authors' Abstract
Narasimha Rao, P. and Lakshmi, T. S. S. Increase of the incidence of dapsone hypersensitivity syndrome-an appraisal. Lepr. Rev. 72(2001)57-62.
There has been an increase in the reports of dapsone hypersensitivity syndrome (DHS) in the past few years, coinciding with the introduction of multidrug therapy (MDT) for leprosy worldwide. The exact cause of this phenomenon is not clear. We report four cases of DHS observed among 252 leprosy patients on MDT and one case of DHS in a patient taking dapsone for nodulocystic acne in the Dermatology Department of the Osmania General Hospital, Hyderabad, India, between June 1997 and January 1999 with few unusual features. In two of these five patients maculo-papular rash was severe and progressed to erythroderma.
Introduction of MDT in 1982 has not only decreased the prevalence of leprosy but also brought about a positive change in the attitude of people which increased the voluntary reporting of leprosy patients. This, coupled with improvements in organization of leprosy control and awareness of DHS among medical personnel, is probably the most important reason for the increased reporting of DHS in recent years.-Authors' Summary
Parizhskaya, M., Youssef, N. N., Di Lorenzo, C. and Goyal, R. K. Clofazimine enteropathy in a pediatric bone marrow transplant recipient. J. Pediatr. 138(2001)574-576.
Clofazimine, previously used in the treatment of leprosy, is now used for treatment of Mycobacterium avium complex infection in patients with acquired immune deficiency syndrome, dermatologie disorders, and graft-versus-host disease. An 11-yearold boy developed a severe enteropathy 2 years after initiation of clofazimine treatment for graft-versus-host disease. Clofazimine enteropathy caused by crystal deposition can be life-threatening.-Authors' Abstract
Suite, M. Relapse rates following leprosy multidrug therapy. West Indian Med. J. 49(2000)210-211.
This is a retrospective study of relapses among leprosy patients who received multiple drug therapy in Trinidad and Tobago between January 1982 and December 1994. The results of the study reveal a relapse rate of 0.65% for multibacillary cases and 1.5% for paucibacillary cases. These results are comparable to the relapse rates reported by the World Health Organization.-Trop. Dis. Bull. 98(2001)93
Terreni, M. and Villani, P. New anti Mycobacterium agents: recent advances in patent literature. Expert Opin. Therapeut. Patents 11(2001)261-268.
Mycobacterium tuberculosis is the greatest single infectious cause of mortality worldwide. In addition disseminated infection with M. avium complex (dMAC) is an increasingly frequent complication in advanced HIV infection. Among the different classes of anU-Mycobacterium compounds studied in the recent years, those of oxazolidinones and imidazole derivatives seem the most likely to provide new useful drugs for the clinical treatment of Mycobacterium infections in the future. Although the most important improvement in the therapy of tuberculosis infections will be obtained using antisense oligonucleotides and vaccines, the research of new "conventional" antituberculous drugs will also remain an important challenge.-Authors' Abstract
CLINICAL SCIENCES
Barbosa, A. M., Martins, E., Jr., Fleury, R. N. and Oproniolla, D. V. A. [One more case of sulfone syndrome.] Hansen. Int. 25(2000)159-162. (in Portuguese)
A case of a patient was reported presenting with fever, pruritus, malaise, and erythroderma surrounding hypochromic macules in the anterior aspect of the trunk after the beginning of the leprosy treatment. Biopsies of lesions showed regular epithelial dermatitis and pleomorphic lymphocytic infiltrate with intense epidermotropism and follicular involvement, bacilli in nerves and macrophages were detected in all the biopsies. Laboratory examinations demonstrated anemia (erythrocytes 3,300,000/mm3; Hb 9.2%) and leukocytosis (20,800 leukocytes/mm3) with 40% of lymphocytes and polymorphism of these cells. These manifestations were labeled as "sulfone syndrome" despite the lack of other components. The authors consider atypical lymphocytosis to be the hallmark of this syndrome and call attention to the lymphocytic pleiomorphism and intense epidermotropism and follicular involvement observed in the histopathological examinations done. This picture disappeared in the subsequent biopsies. They discuss why erythroderma did not involve hypochromic macules of leprosy and consider that an autosensitization phenomena would result in the persistency of the erythroderma even after sulfone was withdrawn.-Authors' English Summary
Fogos, A. R., Oliveira, E. R. A. and Garcia, M. L. T. [Analysis of reasons for treatment dropout-the case of Hansen's disease patients of the Health Unit at Carapina/ES.] Hansen. Int. 25(2000)147-156. (in Portuguese)
The drop out among leprosy patients is a serious problem for public health professionals. This study wishes to analyze the patients' reasons for the default and/or drop out of treatment. It is a retrospective study involving a sample of 42 patients who default and/or drop out of the treatment in the period from 1994 to 1996. It used a semistructure guide of interviews to obtain information. The answers have been grouped in categories of intrinsic reasons and extrinsic reasons that characterize drop out and/or default. The relation between default and drop out was: multibacillary leprosy (MB) 0.8:1; paucibacillary leprosy (PB) 0.7:1. The drop out was justified by intrinsic reasons among PB patients and among MB patients the default was justified by extrinsic reasons. In accordance with the information above deeper work is necessary to orient the Control Program of Leprosy.-Authors' English Summary
Goncalves, G., Goncalves, A., Padovani, C. R. and Parizotto, N. A. [Laser therapy applied to leprous and nonleprous ulcer healing: a clinical trial in outpatient units of the Public Health Service.] Hansen. Int. 25(2000)133-142. (in Portuguese)
Plantar ulcer is a very frequent physical disability caused by leprosy. This fact imposes, to endemic countries, the necessity of applying newer technologies to improve the quality of life of such patients, by developing more resolutive public health services. Aiming to contribute to these objectives, a clinical trial on chronic ulcer healing by laser therapy was conducted, comparing leprous and nonleprous lesions, in local health units. Once the reference population was defined, inclusion and exclusion criteria were established, and ethical norms observed. Measuring, evaluation and application of standardized procedures were adopted, as well as clinical and documental follow up. A set of indicators based on quantitative and qualitative scales has been used, measuring on item width, length, depth and volume; in the same manner, clinical lesion signs were also rigorously considered, as erythema, edema and limits aspects. For statistical analysis, ANOVA, Wilcoxon and Goodman tests (for variations intra and among multinomial populations) were employed. Lesion disappearance prevailed significantly on reduction and worsening among leprosy patients (66.7; 16.7% and 16.7%, respectively) and nonleprosy patients (55.3; 20.0% and 26.7%). This points out not only expansion of therapeutic possibilities to the studied conditions in local public health services, but also to the success of laser therapy in such conditions.-Authors' English Summary
Kuniar, B., Kaur, I., Rai, R., Mandal, S. K. and Sharma, V. K. Involvement of male genitalia in leprosy. Lepr. Rev. 72(2001)70-77.
Four-hundred-sixty-seven male patients with leprosy were screened for genital involvement. Genital lesions were observed in 6.6% of all male cases of leprosy. They were seen most frequently in lepromatous leprosy (25.8%), followed by borderline lepromatous (13.3%) and borderline tuberculoid (1.4%) leprosy.-Authors' Summary
Lemaster, J. W., Shwe, T., Butlin, C. R. and Roche, P. W. Prediction of "highly skin smear positive" cases among MB leprosy patients using clinical parameters. Lepr. Rev. 72(2001)23-28.
Although "highly skin smear positive" MB leprosy cases are known to be at high risk of relapse after release from treatment, and have been recommended to receive "prolonged duration" MDT, government field-based control programs without skin smear facilities have no simple alternative method to detect such cases. This study reports a significant prevalence of "highly smear positive" cases among 2374 new multibacillary cases recently surveyed by skin smears in Nepal, and retrospectively analyzes 555 newly detected, previously untreated BL and LL cases to identify clinical and laboratory parameters that may be associated with a "highly positive skin smear." While some parameters showed high sensitivity in predicting "highly positive smear" status, none showed both high sensitivity and high specificity simultaneously.-Authors' Summary
Lockwood, D. N. and Reid, A. J. The diagnosis of leprosy is delayed in the United Kingdom. QJM 94(2001)207-212.
Diagnostic delay in leprosy can have serious neurological consequences for the patient. We studied the presentation of leprosy patients, focusing on delays in diagnosis, in a retrospective case-note review of 28 patients referred to The Hospital for Tropical Diseases during 1995-1998. The median ages at onset of symptoms and at diagnosis were 25.1 years (range 9-77.7) and 30.1 years (range 9-78.3), respectively. The median time from symptom onset to diagnosis was 1.8 years (0.2-15.2). Prior to referral to a leprologist, patients had seen a dermatologist (20), neurologist (9), orthopedic surgeon (5) and rheumatologist (2). Delay in diagnosis occurred in 82% of cases. Misdiagnoses as dermatological and neurological conditions were important causes of delay, and 68% of patients had nerve damage resulting in disability. Leprosy can be difficult to diagnose outside endemic areas. Increased awareness among general practitioners and hospital specialists would lead to more rapid diagnosis, thus minimizing damage and disability.-Authors' Abstract
Manjunath, R., Kamath, K. N., Pai, G. S., Pinto, J. and Vinod, V. Modified Active Surveillance System (MASS); a novel clinicopathological evaluation of PB leprosy patients after RFT, in Mangalore, India. Lepr. Rev. 72(2001)50-56.
The current recommendations for leprosy control programs include stopping active surveillance in view of the very low relapse rates and a phased integration of leprosy services with the general health services. Passive surveillance may not be adequate, more so because of the introduction of newer, shorter drug regimens. This study is an effort to evolve a modified active surveillance, which is cost-effective, simple and also a novel substitute for the increased workload caused by the dwindling number of PMWs. One thousand one hundred RFTPB leprosy patients were recalled for a review under the Modified Active Surveillance System (MASS), carried out over two phases. Patients were divided into groups as per the mode of response to the mailed postcards: responders (patients who reported to the OPD in person), untraceables (patients whose postcards returned back) and nonresponders (patients who did not report to the OPD after receiving the mail). At the end of phase I, we had 120 responders, 480 untraceables and 500 nonresponders. In phase II, which began 2 months later, the 500 nonresponders were dispatched reminders. In this phase, there were 31 responders, 60 untraceables and 409 nonresponders. Thus, at the completion of phases I and II, there were 151 responders, 540 untraceables and 409 nonresponders. Of the 151 patients examined, 71 had no complaints (category I), 41 had fresh leprosyrelated complaints (category IIA), 14 had fresh leprosy-unrelated complaints (category IIB) and 25 had persistence of old complaints (category III). Cumulative PYR of the 151 patients was 1155.42. Forty-one patients had fresh leprosy-related complaints. Skin biopsy was done in the 17 patients with fresh skin patches, of whom four showed histopathological evidence of relapse. Relapse rate in our study was 0.35/100 PYR. Mean duration after RFT at relapse was 4.9 years. Our skepticism toward passive surveillance systems is justified by these 41 patients with fresh leprosyrelated complaints, who voluntarily reported only after receiving the postcards. We recommend the introduction of a phase III, wherein the services of PMWs may be used to contact the 409 patients who remained unresponsive at the completion of phases I and II. We also recommend the introduction of a universal format for recording addresses of all new patients, which would be of immense help in patient retrieval in all such surveillance systems in the future.-Authors' Summary
Marcos, E. V. C., Ura, S., de Souza, F. C. and Oproniolla, D. V. A. Study of the association of HLA antigens and ulcerated type 1 leprotic reaction. Anais Bras. Dermatol. 75(2000)283-290.
Many important associations between HLA antigens and several diseases have been described, the mechanisms of susceptibility still remain obscure and there is evidence that the same gene locus is not involved with the same mechanism that acts in the different pathologies. Associations studies with leprosy patients with reactions, especially in those with ulcerated type 1 reactions, have not been realized so far. The objective of the present study was to investigate a possible association between HLA antigens class II and ulcerated type 1 leprosy reaction, establishing a comparison with controls of the same ethnic group. HLA-A, B, DR and DQ antigens were determined in 12 patients, 11 of whom had reactive tuberculoid leprosy (MHTR) and 1 patient had reactive borderline leprosy (MHDR). The Caucasoid samples were used as control group in the population of the state of São Paulo (Brazil). HLA antigen frequency comparison between patients and the control group and the control has not shown any kind of association; however, a significant increase was observed in HLA-DR2 antigen frequency (63.3 vs. 19%, p <0.05). In conclusion, our data have not indicated any type of association between HLA antigens and ulcerated type 1 leprosy reaction, but suggest that HLA complex genes may have a role in the development of the clinical form of leprosy.Trop. Dis. Bull. 97 (2000)
Natrajan, M., Katoch, K. and Katoch, W. M. Patients presenting with defined areas of sensory loss-a preliminary study. Indian J. Lepr. 73(2001)17-26.
Thirty patients presenting with circumscribed areas of clearly demonstrable hypesthesia were chosen from among those attending this institute. Their history and clinical features were recorded, lepromin test was done for reading at 4 weeks, and peripheral part of the hypesthetic area was biopsied for histopathology and immunostaining. The subjects were predominantly adult males with the symptomatic sites limited to the extremities. On routine histopathological examination of the symptomatic sites, the diagnosis of leprosy, using defined criteria, could be made in 6 cases (20%). Immunostaining of the remaining sections showing either no pathology or a nonspecific pathology revealed the presence of mycobacterial antigen in 5 of the 24 cases (20.83%). Overall, leprosy could be diagnosed in 11 of the 30 cases studied (36.66%). This study shows that leprosy may be an important cause of circumscribed areas of sensory deficit.-Authors' Abstract
Nery, J. A. C., Sampaio, E. P., Galhardo, M. C. G., Perisse, A. R. S., Vieira, L. M. M., Salles, A. M. and Sarno, E. N. M. leprae-HIV co-infection: pattern of immune response in viva and in vitro. Indian J. Lepr. 72(2000)155-167.
The clinical and histological features of leprosy in 17 patients with Mycobacterium leprae and human immunodeficiency virus co-infection [Brazil, date not given] are described. The development of reversal reaction, both in vitro and in vivo, during positive immune response to M. leprae in co-infected patients are discussed.-Trop. Dis. Bull. 98(2001)921
Paredes, S. N., Cuello, C. and Prida, M. [Study of the knowledge of Hansen's disease by health workers.] Hansen. Int. 25(2000)157-158. (in Portuguese)
Sanitary education in leprosy is considered a priority in a strategy of work to reach the goal of elimination of leprosy launched by the WHO (World Health Organization) for the year 2000. This was the reason that we wanted to enquire the level of knowledge of health workers previous to the development of the courses and the workshops. We introduce here the results of 33 courses, made during 5 years, from 1995 to 1999 inclusive, with 1065 students and their answers to different aspects of leprosy, and an epidemiological correlation based on recorded information.-Authors' English Summary
Ramadan, W., Mourad, B., Fael, W. and Ghoraba, E. Clinical, electrophysiological, and immunopathological study of peripheral nerves in Hansen's disease. Lepr. Rev. 72(2001)35-49.
Hansen's disease is a disease of peripheral nerves. Some patients develop peripheral neuropathy before the diagnosis of the disease, and others develop these complications after starting therapy. Electrophysiological (EP) studies were carried out in Hansen's disease patients. This work studied the neural deficits, electromyography (EMG) and motor nerve conduction (MNC) variables in different types of leprosy and the immunopathology of sural nerve tissue in patients with severe neural deficits. Forty leprosy patients had neurological examinations and EP study. Histopathological and immunopathological study of sural nerve biopsy specimens was performed for 10 patients with severe neural deficits. The results of the neurological study showed that there was involvement of cranial nerves, muscular system, motor reflexes and sensory system and trophic and vasomotor changes. EP study showed significant changes in EMG of abductor digiti minimi in patients as compared to controls. MNC variables of common peroneal nerve were abnormal in 80% of all patients, MNC of median nerve was abnormal in 72.5%, while MNC of ulnar nerve was abnormal in 70% and SNC of ulnar nerve was abnormal in 77.5% of the total. In conclusion, electrophysiological investigations have an important role in the detection of muscle denervation and neuropathic changes in leprosy patients. These investigations are safe, rapid and noninvasive techniques. On the other hand, immunopathological study revealed that the degree of immune positivity correlated with the degree of nerve fibrosis.Authors' Summary
Ramu, G. Clinical leprosy through the last seventy-five years. Indian J. Lepr. 72(2000)199-214.
A review of the clinical aspects of leprosy through the pre-sulfone, sulfone and multiple drug therapy era is presented. The regional variations, diagnosis, evolution and classification of leprosy, and the occurrence of relapses and co-infection with tuberculosis and human immunodeficiency virus infection are discussed.-Trop. Dis. Bull. 98(2001)925
Ruzzenenti, M. R., Bruni, R., Florio, G., De Luigi, M. C., Lercari, G., Barabino, G. F., Nunzi, E. and Valbonesi, M. Lepromatous vasculitis successfully treated by plasma exchange (PE). J. Clin. Apheresis 16(2001)37-38.
Vascular involvement is presently considered a "common pathway" in a number of diseases that are mediated by circulating immune complexes (CIC). CIC are found in the circulation when the disease is active and in single patients their level may parallel disease activity. Lepromatous leprosy is characterized by the presence of CIC and deposits of immunoglobulins and complement in vascular lesions of the different organs and an Arthus-like mechanism is considered as the basis for the clinical picture. The same mechanism is considered to play an essential pathophysiologic role in Lucio's phenomenon, which is characterized by lymphohistiocytic vascular infiltrates with or without thrombosis and secondary cutaneous infarction. Lepromatous vascular involvement is mediated by CIC whose antigen composition is known, the same as it is with HCV mediated cryoglobulinemia, HBV positive panarteritis nodosa, rheumatoid vasculitis, or Wagner's granulomatosis, which are usually treated by PE. PE has been employed for lepromatous vasculitis since 1979 and other cases have been successfully treated afterward. We report on another patient successfully treated by plasma exchange.-Authors' Abstract
Saunderson, P. The epidemiology of reactions and nerve damage. Lepr. Rev. 71 Suppl.(2000)S106-S110.
The ALERT MDT Field Evaluation Study (AMFES) in Ethiopia, which was begun in 1988, involves the follow up of 594 new patients for as long as 10 years after completion of treatment, including 6 month assessments of nerve function. In contrast to similar studies in India and Bangladesh, the Ethiopian cohort presented late, had a high rate of disability at diagnosis (55%), a high rate of multibacillary disease (51%) and a high rate of subsequent neuropathy (43%). Preliminary findings include the following. One-third of the patients never exhibited nerve damage. True acute neuropathy has a very good prognosis when treated with a standard course of steroids; full recovery was observed in 88% of nerves. Chronic and recurrent neuropathy have a worse prognosis; these problems need to be identified early and managed appropriately, employing either new steroid regimens or new drugs. The risk factors identified in this study include, for neuropathy, older age, delay of diagnosis, thickened nerves at diagnosis, and reversal reactions. Risk factors for chronic or recurrent neuropathy include classification, impairment at diagnosis, and reversal and ENL reactions. Those factors associated with a poor outcome include impairment at diagnosis, and chronic or recurrent neuropathy. Various problems faced in research in the area of leprosy reactions and neuropathy are discussed, as are the priorities for research in the future.-Author's Summary
Shetty, V. P., Mistry, N. F. and Antia, N. H. Current understanding of leprosy as a peripheral nerve disorder: significance of involvement of peripheral nerve in leprosy. Indian J. Lepr. 72(2000)339-350.
A paper discussing the mechanism of nerve damage in leprosy, predilection of Mycobacterium leprae for peripheral nerves, two types of reactions (reversal reaction and erythema nodosum leprosum) and nerve damage, and the restoration of nerve function in leprosy patients is presented.'Trop. Dis. Bull. 98(2001)1692
Smith, W. C. S. Review of current research in the prevention of nerve damage in leprosy. Lepr. Rev. 71 Suppl.(2000)S138-S145.
Nerve damage and the consequences of nerve damage set leprosy apart from other diseases. The irreversible motor and sensory impairments caused by leprosy lead to increasing secondary impairments long after the disease process has been arrested. Interventions that prevent, reverse or limit the impairments resulting from leprosy are, therefore, of the highest priority. Self-care has been demonstrated to be an effective means of preventing secondary tissue damage, and its implementation must now be encouraged within the framework of basic health care. Currently, a comprehensive effort has been made to address all dimensions of impairment of nerve function and its consequences, from prevention of both primary and secondary impairments to interventions in long-term nerve damage. The BANDS prospective study of a cohort of 2664 previously untreated leprosy patients in Bangladesh has provided both a valuable baseline and insight into the epidemiology of nerve damage in leprosy. This work has defined the numbers of patients who present with acute nerve damage, the numbers who are not treated, and the importance of the MB classification, and has described the simple clinical prediction rule. This study also provided the basis for the development of the three TRIPOD randomized clinical trials in Nepal and Bangladesh. Follow up of the BANDS cohort, which is continuing, will yield more data on the natural history of nerve damage. The encouraging results from the TRIPOD trials of low-dose prophylactic steroids will be followed up to see whether the effect is sustained over time. The TRIPOD trials are to be completed, a trial of three steroid regimens in reversal reaction is to be completed, and a number of specific research topics within the ILEP program, INFIR, are to be developed.-Author's Summary
van Brakel, W. H. Detecting peripheral nerve damage in the field: our tools in 2000 and beyond. Indian J. Lepr. 72(2000)47-64.
Apart from early detection of leprosy and prompt treatment with multidrug therapy, nerve function assessment (NFA) and steroid treatment of any impairment detected are the main methods of primary prevention of" impairment and disability. This review provides a table of available instruments and tests to assess peripheral nerve function and discusses the simplicity and efficacy of the different tests. Conclusions and recommendations are given.-Trop. Dis. Bull. 98(2001)4292
von Brakel, W. H. Peripheral neuropathy in leprosy and its consequences. Lepr. Rev. 71 Suppl.(2000)S146-S153.
Leprosy causes a "mononeuritis multiplex" of immunological origin that results in autonomic, sensory and motor neuropathy. When detected and treated early, primary impairments may be reversible. However, 11 %-51 % of patients do not recover. In addition, 33%-56% of newly registered patients already have clinically detectable impairments, often no longer amenable to drug treatment. Among new patients, 6%-27% present with secondary impairments, such as wounds, contractures and shortening of digits. All patients with impairments should be taught methods to prevent further impairment and subsequent disability (POID). As the result of impairments, many people experience limitation of activities of daily living, which can be partially overcome with the help of assistive devices, training, and surgery. As a result of these limitations, because of visible impairments, or simply because of the diagnosis "leprosy," many people are restricted in their participation in society. Many overcome activity limitations and participation restrictions without assistance, despite residual impairments. However, some require intervention, such as physical or occupational therapy, reconstructive surgery or temporary socioeconomic assistance. Information on these issues is not collected routinely, and the few tools that exist to measure the severity or extent of impairment have not been widely used, nor have they been used to generate cohort-based statistics. There are no agreed indicators for monitoring POID activities or rehabilitation interventions. Work in the general field of rehabilitation has resulted in the ICIDH-2, which provides a conceptual framework for rehabilitation and the entire area of "consequences of health conditions." Although experience to date is very limited, the conceptual framework appears appropriate to leprosy. Data on the prevalence and incidence of primary and secondary impairments have been reported from several countries, the link between impairments and activity limitations has been investigated, and a few studies of the magnitude of the need for rehabilitation have been reported. Research priorities include studies of methods to improve detection of autonomic, sensory and motor neuropathy; trials of alternative drugs or regimens for treating neuropathy; studies of the use of various POID-monitoring systems that may be derived from these; studies of the design and use of instruments to assess limitations of activities and restrictions on participation; assessments of needs for rehabilitation and the development of methods to do these; studies of the efficacy of various types of rehabilitation interventions for particular conditions; and studies of the cost-effectiveness of such interventions.-Author's Summary
Welsh, O., Gomez, M., Mancias, C., Ibarra-Leal, S. and Millikan, L. E. A new therapeutic approach to type 2 leprosy reaction. Int. J. Dermatol. 38(1999)931-933.
Clofazimine and pentoxifylline were evaluated for their efficacy against severe type 2 leprosy reaction in 4 patients (3 men and 1 woman) from Mexico. All 4 patients showed a similar fast response to treatment. It is concluded that the results obtained in this study are promising; however, clofazimine and pentoxifylline must be evaluated in a larger group of patients in order to determine their value in controlling type 2 leprosy reaction.-Trop. Dis. Bull. 97(2000)4285
IMMUNO-PATHOLOGY
Beatty, W. L., Ullrich. H.J. and Russell, D. G. Mycobacterial surface moieties are released from infected macrophages by a constitutive exocytic event. Eur. J. Cell Biol. 80(2001)31-40.
Bacterial cell wall constituents are released from mycobacterial phagosomes and actively traffic within infected macrophages. Colocalization of fluorescently tagged bacterial moieties with endocytic tracers revealed the dynamic movement of released mycobacterial constituents into the endocytic network with accumulation in tubular lysosomal-like compartments. The released bacterial constituents not only penetrated the infected host cell but were also present in an extracellular microvesicular fraction. To identify the intracellular source of these exocytic compartments, released vesicular material was isolated from culture supernatants by differential ultracentrifugation and characterized by Western blot and electron microscopy analyses. The presence of lysosomal membrane proteins and lysosomal proteases suggested that labeled mycobacterial cell wall constituents access a constitutive lysosomal exocytic pathway. An abundance of multilamellar extracellular compartments morphologically reminiscent of MHC class II-enriched compartments (MI1C) implicated a MHC class II transport pathway in the extracellular release of bacterial constituents. Increases in intracellular free calcium have previously been shown to trigger lysosomal exoeytosis by inducing fusion of lysosomes with the plasma membrane. To test if an increase in calcium would stimulate exoeytosis with release of mycobacterial constituents, infected macrophages were exposed to the calcium ionophore A23187. The ionophore triggered the release of a microvesicular fraction containing labeled bacterial moieties, implicating calcium-regulated lysosomal exoeytosis as a trafficking pathway by which mycobacterial products are released from infected macrophages.-Authors' Abstract
Bermudez, L. E. and Sangari, F. J. Cellular and molecular mechanisms of internalization of mycobacteria by host cells. Microbes Infect. 3(2001)37-42.
Mycobacteria are intracellular pathogens capable of invading mononuclear phagocyte, mucosal epithelial cells (including M cells) and Schwann cells. To enter cells, mycobacteria have been shown to interact with several molecules on macrophage and epithelial cell surfaces. This suggests adaptation to the host environment. In this review we address the strategies used by pathogenic mycobacteria to gain access to the intracellular environment.-Authors' Abstract
Bhake, A. S., Desikan, K. V. and Jajoo, U. N. Cytodiagnosis of histoid leprosy. Lepr. Rev. 72(2001)78-82.
This paper presents cytomorphological features of the histoid variety of lepromatous leprosy. Fine needle aspiration of a lepromatous nodule showed cytological features consistent with those of histoid leprosy. Simultaneously, a biopsy of the nodule was also performed and the case confirmed as histoid leprosy. The advantages of the fine needle aspiration technique are that it is simple, quickly reportable, and less traumatizing. Multiple aspirations from different sites may be obtained, which would add to the value of sampling. The need to differentiate a histoid nodule from a conventional lepromatous nodule is explained.-Authors' Summary
Britton, W. J., Martin, E., Kamath, A. T., Neupane, K. D. and Roche, P. W. Immunoprophylaxis against Mycobacterium leprae infection with subunit vaccines. Lepr. Rev. 71 Suppl.(2000)S176-S181.
We have investigated the effect of subunit vaccines against infection with Mycobacterium leprae, employing DNA plasmids as the vaccine vectors, and the immunodominant 35 kDa protein of M. leprae as the candidate antigen. A DNA vaccine that expresses the M. leprae 35-kDa protein both stimulated interferon-gamma (IFN-γ)secreting T cells in mice, and demonstrated protection against M. leprae infection of mice.-Authors' Summary
Charlab, R., Sarno, E. N., Chatterjee, I). and Pessolani, M. C. V. Effect of unique Mycobacterium leprae phenolic glycolipid-I (PGL-I) on tumour necrosis factor production by human mononuclear cells. Lepr. Rev. 72(2001)63-69.
Mycobacterium leprae cell wall-associated components are found in large amounts in the tissues of leprosy patients, particularly those at the lepromatous pole. Among these molecules, the phenolic glycolipid-I (PGL-I), unique to M. leprae, has been involved in the selective anergy observed in the lepromatous patients. Armadillo-derived M. leprae retains only a small proportion of the total PGL-I found in infected tissues. Therefore, the addition of PGL-I to M. leprae in vitro is important for a better understanding of M. leprae effects in vivo. We have studied the influence of PGL-I on TNF production by normal human peripheral blood mononuclear cells (PBMC) and by a human monocytic leukemia cell line (THP-1) following stimulation with killed M. leprae. PGL-I alone did not induce TNF secretion by PBMC, but when associated with a suboptimal dose of armadillo-derived M. leprae increased the release of this cytokine. In agreement with these results, M. lepraeexposed THP-1 cells did not secrete detectable levels of TNF unless PGL-I was simultaneously added to the culture. This increase in TNF production suggest that PGL-I plays a role in the induction of TNF during the natural infection. In addition, the modulatory effect of PGL-I 011 TNF release by THP-1 cells reinforces that monocytes are one of the possible targets of this molecule .-A u I hors 'Summary
Convit, J. and Ulrich, M. Immunotherapy and immunoprophylaxis of leprosy. Indian J. Lepr. 72(2000)21-32.
This review evaluates the status of immunotherapy and immunoprophylaxis in the treatment and prevention of leprosy, with an emphasis on experience in Venezuela.-Trop. Dis. Bull. 97(2000)4290
Dockell, H. M., Black, G. F„ Weir, R. E. and Fine, P. E. M. Whole blood assays for interferon-y: practicalities and potential for use as diagnostic tests in the field. Lepr. Rev. 71 Suppl.(2000)S60-S62.
Recent years have seen the introduction of a number of whole-blood assays, in which unseparated heparinized blood is stimulated with antigen either overnight or for as long as 6 days, and cytokine production is measured in the plasma or supernatant. These assays have potential for use in the field as immunodiagnostic assays as they require only a small blood sample and basic laboratory facilities. Use of these assays in a large study of the immunological effects of BCG vaccination in Malawi has shown that the diluted blood, 6-day wholeblood assay is robust, and can be used to assess T-cell responses to both crude and recombinant antigens. If used with antigens specific to Mycobacterium leprae, these assays could be used to measure exposure to M. leprae within communities or populations, or to aid the early diagnosis of leprosy.-Authors' Summary
Krahenbuhl, J. and Adams, L. B. Exploitation of gene knockout mice models to study the pathogenesis of leprosy. Lepr. Rev. 71 Suppl.(2000)SI70-S175.
Shepard's technique for growth of Mycobacterium leprae in the mouse foot pad, described in I960, and more recent studies in thymectomized-irradiated mice and rats, athymic nude mice, nude rats and severe combined immunodeficiency (SCID) mice have defined the role of T-cell mediated immunity (CMI) in leprosy. However, the normal mouse and the immunocompromised mouse and rat represent only elements of polar tuberculoid disease and polar lepromatous leprosy, respectively. Transgenic, knockout (KO) mice may be employed to study the roles of individual genes in the ability of the host to mount an effective immune response to pathogens, and may also allow development of mouse models for the immunologically unstable borderline areas of the spectrum. We are exploiting certain KO mice to improve our understanding of CMI to M. leprae, and to study the role of the microenvironment of the leprosy granuloma in pathogenesis. CGD (chronic granulomatous disease) mice and iNOS-KO mice lack the ability to produce reactive oxygen intermediates (ROI) and reactive nitrogen intermediates (RNI), respectively; whereas the T cells of GKO mice are unable to produce interferon-gamma (IFNy). iNOS-KO mice exhibit an enhanced capacity to form granulomas, and the histopathology of the infected foot pad tissues of this strain share many elements of borderline tuberculoid disease. The macrophages of CGD mouse kill or inhibit multiplication of M. leprae, although they lack ROI. Multiplication of the organisms in the foot pad is enhanced in GKO mice, although these mice retain some host resistance. In addition, we have been investigating supplementary, conditional approaches to KO mouse models. For example, the down-regulatory effects of local prostaglandin production can be controlled with essential fatty acid deficient diets or indomethacin, RNI can be blocked in CGD and GKO mice by treatment with aminoguanidine, N<; monomethyl arginine or N(,(l-iminoethyl)-L-lysine, and local elaboration of TNFa can be neutralized by anti-TNFa antibody or excess TNFa receptor. Other cytokines can be neutralized by antibody as well, broadening the range of conditional knockout models.-Authors' Summary
Little, D., Khanolkar-Young, S., Coulthart, A., Suneetha, S. and Lockwood, D. N. Immunohistochemical analysis of cellular infiltrate and gamma interferon, interleukin-12, and inducible nitric oxide synthase expression in leprosy type 1 (reversal) reactions before and during prednisolone treatment. Infect. Immun. 69(2001)3413-3417.
The effects of prednisolone treatment on the cellularity and cytokine (gamma interferon. interleukin-12, and inducible nitric oxide synthase) profiles of leprosy skin type I (reversal) reactions were studied using immunohistochemistry. Skin biopsies were taken from 15 patients with leprosy type 1 (reversal) reactions at days 0, 7, 28, and 180 after the start of steroid treatment. Prednisolone treatment had little effect at day 7, but by day 28 significant decreases were found in cytokine levels. Some patients maintained cytokine production at days 28 and 180. These results illustrate the strong Th1 profile of type 1 reactional lesions, the slow response to steroid therapy, and continuing activity at 180 days.-Authors' Abstract
Lockwood, D. N. J. Steroids in leprosy type 1 (reversal) reactions: mechanisms of action and effectiveness. Lepr. Rev. 71 Suppl.(2000)S111-S114
Steroids are widely sued for the treatment of leprosy reactions. The effectiveness of steroid treatment is variable, with only 60% of patients regaining nerve function. Sequential skin biopsy specimens, obtained from 15 patients with type 1 (reversal) reactions, have been studied to document the cytokine profile and cellularity of the lesions. All of the patients were placed on a standard course of steroids after the first biopsy. Subsequent biopsies were performed 7, 28 and 180 days later. The specimens were stained for interferon-gamma (IFN-γ), interleukin-12 (IL-12) and inducible nitric oxide synthase (iNOS). After the first biopsy, all patients were placed on a standard reducing course of steroids beginning at 30 mg daily. By day 7, treatment with prednisolone showed little effect on the cellularity and cytokine profiles. However, by day 28, significant decreases of IFN-γ, IL-12 and iNOS were found for most patients. Some patients maintained cytokine production at day 28 and even at day 180. These data illustrate the strong Th1 profile of type 1 reactional lesions, the relatively slow response to therapy, and the continuing activity after treatment with steroids for 180 days. The variation of individual responses emphasizes their importance. Additional prospective studies will be required to determine whether patients with high intralesional levels of cytokine are at risk of recurrent reactions. The need for studies both of different glucocorticoids and of other nonsteroidal immunosuppressants for the treatment of reactions is discussed.-Author's Summary
Macfarlane, A., Mondragon-Gonzalez, R., Vega-Lopez, F., Wieles, B., de Pena, J., Rodriguez, O., Suarez, Y., De La Torre, R., de Vries, R. R., Ottenhoff, T. H. and Dockrell, H. M. Presence of human T-cell responses to the Mycobacterium leprae 45-kilodalton antigen reflects infection with or exposure to M. leprae. Clin. Diasin. Lab. Immunol. 8(2001)604-611.
The ability of the 45-kDa serine-rich Mycobacterium leprae antigen to stimulate peripheral blood mononuclear cell (PBMC) proliferation and gamma interferon (IFN-γ) production was measured in leprosy patients, household contacts, and healthy controls from areas of endemicity in Mexico. Almost all the tuberculoid leprosy patients gave strong PBMC proliferation responses to the M. leprae 45-kDa antigen (92.8%; N = 14). Responses were lower in lepromatous leprosy patients (60.6%; N = 34). but some responses to the 45-kDa antigen were detected in patients unresponsive to M. leprae sonicate. The proportion of positive responses to the M. leprae 45-kDa antigen was much higher in leprosy contacts (88%; N = 17) than in controls from areas of endemicity (10%; N = 20). None of 15 patients with pulmonary tuberculosis gave a positive proliferation response to the 45kDa antigen. The 45-kDa antigen induced IFN-γ secretion similar to that induced by the native M. tuberculosis 30/31-kDa antigen in tuberculoid leprosy patients and higher responses than those induced by the other recombinant antigens (M. leprae 10and 65-kDa antigens, thioredoxin, and thioredoxin reductase); in patients with pulmonary tuberculosis it induced lower IFN-γ secretion than the other recombinant antigens. These results suggest that the M. leprae 45-kDa antigen is a potent T-cell antigen which is M. leprae specific in these Mexican donors. This antigen may therefore have diagnostic potential as a new skin test-reagent or as an antigen in a simple whole-blood cytokine test.-Authors' Abstract
Martin, E., Roche, P. W., Triccas, J. A. and Britton, W. J. DNA encoding a single mycobacterial antigen protects against leprosy infection. Vaccine 19(2001)1391-1396.
The continuing incidence of leprosy infection around the world and the inability of Mycobacterium bovis bacille CalmetteGuerin (BCG) to protect certain populations clearly indicates that an improved vaccine against leprosy is needed. The immune dominant 35-kDa protein, shared with M. leprae and M. avium, but not M. tuberculosis or BCG, is recognized by >90% of leprosy patients, making it an ideal candidate antigen for a subunit vaccine. Immunization of outbred Swiss albino mice with a DNA-35 vaccine stimulated specific T-cell activation and IFN-gamma production. DNA-35 immunization induced significant levels of protection against M. leprae foot pad infection, comparable to that produced by BCG. Therefore, DNA immunization with the 35-kDa antigen is effective against M. leprae infection and genetic immunization with a combination of antigens holds the potential for an improved vaccine against leprosy.-Authors' Abstract
McShane, H., Brookes, R., Gilbert, S. C. and Hill, A. V. S. Enhanced immunogenicity of CD4+ T-cell responses and protective efficacy of a DNA-modified vaccinia virus Ankara prime-boost vaccination regimen for murine tuberculosis. Infect. Immun. 69(2001)681-686.
DNA vaccines whose DNA encodes a variety of antigens from Mycobacterium tuberculosis have been evaluated for immunogenicity and protective efficacy. CD8+ T-cell responses and protection achieved in other infectious disease models have been optimized by using a DNA immunization to prime the immune system and a recombinant virus encoding the same antigen(s) to boost the response. A DNA vaccine (D) and recombinant modified vaccinia virus Ankara (M) in which the DNA encodes early secreted antigenic target 6 and mycobacterial protein tuberculosis 63 were synthesized, and each was found to generate specific gamma interferon (IFN-γ)-secreting CD4+T cells. Enhanced CD4+ IFN-γ T-cell responses were produced by both D-M and M-D immunization regimens. Significantly higher levels of IFN-γ were seen with a D-D-D-M immunization regimen. The most immunogenic regimens were assessed in a challenge study and found to produce protection equivalent to that produced by M. bovis BCC. Thus, heterologous prime-boost regimens boost CD4+ as well as CD8+ T-cell responses, and the use of heterologous constructs encoding the same antigen(s) may improve the immunogenicity and protective efficacy of DNA vaccines against tuberculosis and other diseases.-Authors' Abstract
Moraes, M. O., Sampaio, E. P., Nery, J. C., Saraiva, B. C. C., Alvarenga, F. F and Sarno, E. N. Sequential erythema nodosum leprosum and reversal reaction with similar lesional cytokine mRNA patterns in a borderline leprosy patient. Br. J. Dermatol. 144(2001)175-181.
We compare the clinical and histological data with the immunological status of a borderline leprosy patient who experienced an erythema nodosum leprosum (ENL) reaction followed by a reversal reaction (RR) after 12 weeks of anti-inflammatory treatment [pentoxifylline (PTX) 1200 mg daily]. Skin biopsies, serum and blood samples were collected sequentially during the reactional episodes. At the outset of RR, the patient's lymphocytes secreted interferon gamma (IFN-γ) and there was a positive lymphoproliferative test in response to Mycobacterium leprae, which had been absent during ENL. The lepromin reaction reversed from negative (0 mm) at diagnosis to positive (3 mm) 3 months after the development of RR. Tumor necrosis factor alpha (TNF-α) levels in the serum decreased after 1 week of treatment and increased slightly thereafter. The immunohistochemical data for ENL showed a diffuse dermal and hypodermal infiltrate composed of mononuclear cells and neutrophils, while RR was characterized by an epithelioid granulomatous infiltrate with a marked presence of gamma delta T cells. Reverse transcription-polymerase chain reaction showed a mixed cytokine profile characterized by the expression of TNF-α, IFN-γ, interleukin (IL)-6, IL-10 and IL-12 mRNA in the skin, which persisted throughout the development of ENL and RR lesions. IL-4 mRNA, first detected after 7 days of PTX treatment, was still present during RR. The results suggest the emergence of an initial ThO-like cytokine profile in ENL, typical of a state of immunoactivation, before conditions optimal for the appearance of an antigen-specific cell-mediated immune response and gamma delta T-cell migration are created.-Authors' Abstract
Mysorekar, V. V., Dandekar, C. P. and Rao, S. G. Mast cells in leprosy skin lesions. Lepr. Rev. 72(2001)29-34.
The density and distribution of mast cells was assessed in skin biopsies of 188 untreated leprosy cases and 20 healthy individuals taken as controls. Mast cells were present in only small numbers in the skin biopsies of healthy individuals. Significantly higher mast cell counts were obtained in the skin lesions of indeterminate leprosy (p <0.01). The mast cell count in the tuberculoid group was significantly lower than that in the lepromatous group (p <0.05). The lepromatous group also showed increased mast cell degranulation and altered morphology. The mast cell distribution in the skin biopsies of the two groups was, however, similar. The mast cell count in leprosy is probably determined by the pattern of cytokines released by the T lymphocytes. However, the influence of mast cells on the outcome of the disease needs to be evaluated further.-Authors' Summary
Nath, I., Vemuri, N., Reddi, A, L., Bharadwaj, M., Brooks, P., Colston, M. J., Misra, R. S. and Ramesh, V. Dysregulation of IL-4 expression in lepromatous leprosy patients with and without erythema nodosum leprosum. Lepr. Rev. 71 Suppl.(2000)S130-S137.
In order to increase our understanding of the immunological basis of erythema nodosum leprosum (ENL), we studied Th-like cytokine profiles in 130 leprosy patients, employing both the conventional and a novel, real-time, fluorogenic reverse transcriptase-based PCR (RT-PCR). The concomitant expression of both Th-like cytokines, interferon gamma (IFN-γ) and IL4, and the regulatory cytokines, IL-10 and IL-12, was studied in the peripheral blood cells of leprosy patients with and without ENL. In the conventional RT-PCR, varied cytokine profiles were observed in individual patients of all clinical types. Fifty-three percent of lepromatous patients without ENL and 59% of tuberculoid leprosy patients showed co-expression of IFN-γ and IL-4, indicating a nonpolarized ThO pattern. Of the 36 patients with ENL, 58% demonstrated a polarized Th1 pattern, with only 30% expressing both cytokines. Semiquantitative RT-PCR indicated a lower expression of IL-4 compared to that of IFN-γ in the lepromatous patients without ENL; the difference was even greater among those with ENL. The sensitive, real-time PCR confirmed the down-regulation of IL-4 and IL-10, with absence of IL-4 in half of the patients, resulting in skewing of the cytokine response toward a Till-like profile.-Authors' Summary
Ochoa, M. T., Stenger, S., Sieling, P. A., Thoma-Uszynski, S., Sabet, S., Cho, S. G., Krensky, A. M., Rollinghoff, M., Sarno, E. N., Burdick, A. E., Rea, T. H. and Modlin, R. L. T-cell release of granulysin contributes to host defense in leprosy. Nature Med. 7(2001)174-179.
A novel mechanism by which T cells contribute to host defense against microbial pathogens is release of the antimicrobial protein granulysin. Wc investigated the role of granulysin in human infectious disease using leprosy as a model. Granulysinexpressing T cells were detected in cutaneous leprosy lesions at a sixfold greater frequency in patients with the localized tuberculoid as compared with the disseminated lepromatous form of the disease. In contrast, perforin, a cytolytic molecule that colocalizes with granulysin in cytotoxic granules, was expressed at similar levels across the spectrum of disease. Within leprosy lesions, granulysin colocalized in CD4+ T cells and was expressed in CD4+ T-cell lines derived from skin lesions. These CD4+ T-cell lines lysed targets by the granule exocytosis pathway and reduced the viability of mycobacteria in infected targets. Given the broad antimicrobial spectrum of granulysin, these data provide evidence that T-cell release of granulysin contributes to host defense in human infectious disease.-Authors' Abstract
Ochoa, M. T., Thoma-Uszynski, S., Sieling, P. A., Sabet, S., Cho, S., Krensky, A. M., Burdick, A., Rea, T. H. and Modlin, R. L, Role of granulysin in immunity to leprosy. Lepr. Rev. 71 Suppl.(2000)SI15-S116.
One component of human T-cell cytotoxic granules, granulysin, exhibits a broad spectrum of activity against microbial pathogens. We investigated the role of granulysin in human infectious diseases, employing leprosy as a model. Expression of granulysin was detected in cutaneous leprosy lesions six times more frequently among patients with localized than among those with disseminated disease. Granulysin co-localized in CD4+ T cells within leprosy lesions as well as in CD4+ T-cell clones derived from lesions. These CD4+ T cells lysed targets by means of the granule exocytosis pathway, and reduced the viability of both Mycobacterium tuberculosis and M. leprae in infected targets. These data indicate a direct effector function of CD4+ T cells that is mediated through their ability to secrete the antimicrobial protein, granulysin, at the site of the infection.
We also determined the distribution and frequency of granulysin in reactional states in leprosy. We found that expression of granulysin was greater among patients with reversal reactions than among those with erythema nodosum leprosum, and was least frequent among lepromatous patients who were not in reaction. These results suggested that granulysin can also contribute to bacterial killing during reactional states or lead to the tissue-injury typical of these reactions.-Authors' Summary
Ranibukkana, A. Molecular basis for the peripheral nerve predilection of Mycobacterium leprae. Curr. Opin. Microbiol. 4(2001)21-27.
Mycobacterium leprae, the causative organism of leprosy, has a unique predilection for Schwann cells, the glial cclls of the peripheral nervous system. M. leprae invasion of Schwann cells leads to the neurological damage that underlies the sensory motor loss and subsequent deformity and disability associated with this disease. Recent studies have begun to elucidate the early events of M. leprae infection of Schwann cells on a molecular level, and the host and bacterial factors that determine the neural predilection of this bacterium. These advances have now provided novel insights into the mechanisms of bacterial interactions with host cells.-Authors' Abstract
Santos, D. O., Santos, S. L., Esquenazi, D., Nery, J. A., Defruyt, M., Lorre, K. and Van Heuverswyn, H. Evaluation of B7-1 (CD80) and B7-2 (CD86) costimulatory molecules and dendritic cells on the immune response in leprosy. Jpn. J. Hansen's Dis. 70(2001)15-24.
The cell activation depends on T-cell antigen receptor binding to antigen plus MHC and costimulation. The binding of CD28, expressed on the T-cell surface to B7 (B7-1 or CD80/B7-2 or CD86) present on the antigen-presenting cells (APCs), determines, in several T-cell function models, if activation or anergy follows antigenic stimulation. In leprosy, the role of CD80 and CD86 as costimulatory signal in M. leprae specific cellular immunity has not yet been defined. We investigated the role of B7CD28 pathway of T-cell activation in the in vitro response to M. leprae following stimulation in the presence of monocytes or dendritic cells (DCs) as APCs. Monocytes were purified, by cold aggregation, from peripheral blood mononuclear leukocytes (PBMC) isolated from leprosy patients. In order to obtain DCs, the monocytes were cultured in the presence of ID-4 and GMCSF. T cells were purified from PBMC by negative selection with mABs and C'. The phenotype of the cell populations was monitored by FACS. Lymphoproliferative assays were performed with T cells in the presence of monocytes or DCs. The cells were stimulated by M. leprae in the presence of anti-CD80 antibody (Ab) and/or anti-CD86 antibody (Ab) (Innogenetics). In some experiments IL-10, IL-12 and anti-IL12 Ab were also added to the culture. We observed a significantly more efficient APC function for DCs when compared to monocytes in T-cell in vitro responses to M. leprae. Regardless of the clinical form of leprosy, the M. leprae-specific immune response was markedly reduced in the presence of anti-CD86 Ab. IL-12 increases the immune response to M. leprae while IL10 or anti-IL-12 Ab reduce this response when monocytes or DCs were used as APCs.-Authors' Abstract
Sarno, E. N., Santos, A. R., Jardim, M. R., Suffys, P. N., Almeida, A. S., Nery, J. A. C., Vieira, L. M. M. and Sampaio, E. P. Pathogenesis of nerve damage in leprosy: genetic polymorphism regulates the production of TNF-α. Lepr. Rev. 71 Suppl.(2000)S154-S160.
Studies carried out over the last decade have strongly suggested that tumor necrosis factor alpha (TNF-α) both overtly participates in the cell-mediated immune response against Mycobacterium leprae, and is overproduced during reaction. In addition, reactions are intimately related to the onset of nerve damage. Finally, TNF-α has been implicated in the pathogenesis of many human and experimental autoimmune peripheral neuropathies that, as in leprosy, result in demyelination and axonal lesions. Because of recent findings associating human TNF-α mutant alleles at the -308 position with increased production of TNF-α in many immunological and infectious diseases, an investigation of the role ofTNF-2 in predisposing leprosy patients to reaction has been undertaken. Analysis of 300 patients with leprosy-210 multibacillary and 90 paucibacillary-has shown that the percentage of reactional patients was similar among both carriers and noncarriers of the TNF-2 allele. However, a separate analysis of 57 carriers of TNF-2 found that reactions occurred much more frequently among heterozygous than among homozygous patients. Moreover, the frequency of neuritis was somewhat greater among the heterozygous patients than among the noncarriers. Enhanced serum levels of TNF-α have been noted in both TNF-1 and TNF-2 mutant patients in the course of leprosy reaction. Our observations to date suggest that other factors not related to the presence of the mutant gene may lead to the TNF-α hyper-responsiveness observed during reaction.-Authors' Summary
Scollard, D. M. Endothelial cells and the pathogenesis of lepromatous neuritis: insights from the armadillo model. Microbes Infect. 3(2000)1835-1843.
Selective infection of peripheral nerves is a unique property of Mycobacterium leprae that results in serious injury, but its basis is unexplained. Recent evidence from infected armadillos suggests that endothelial cells of peripheral nerve vasculature may be (lie gatekeepers by which M. leprae inlects nerves. The pathogenesis of neuropathy in leprosy may thus entail a dynamic sequence of adhesion, immunologic, and inflammatory processes involving peripheral nerve endothelial cells.-Author's Abstract
Scngupta, U. Immunopathology of leprosy-current status. Indian J. Lepr. 72(2000)381-391.
A review discussing the mode of entry of Mycobacterium leprae in humans, immunohistochemical picture of lesions, immunological environments in epidermis and granuloma, dynamics of T-cell functions, functions of T-cell subsets in relation to their cytokine secretion, role of γδ and a(5 T cells in early infection with a pathogen and the immunopathology of reactions in leprosy is presented.-Trop. Dis. Bull. 98(2001)1695
Siddiqui, M. R., Meisner, S., Tosh, K., Balakrishnan, K., Ghei, S., Fisher, S. E., Golding, M., Shanker Narayan, N. P., Sitaraman, T., Sengupta, U., Pitchappan, R. and Hill, A. V. A major susceptibility locus for leprosy in India maps to chromosome 1 Op 13. Nat. Genet. 27(2001)439-441.
Leprosy, a chronic infectious disease caused by Mycobacterium leprae, is prevalent in India, where about half of the world's estimated 800,000 cases occur. A role for the genetics of the host in variable susceptibility to leprosy has been indicated by familial clustering, twin studies, complex segregation analyses and human leukocyte antigen (HLA) association studies. We report here a genetic linkage scan of the genomes of 224 families from South India, containing 245 independent affected sibpairs with leprosy, mainly of the paucibacillary type. In a two-stage genome screen using 396 microsatellite markers, we found significant linkage [maximum lod score (MLS) = 4.09, p <2 x 10-5] on chromosome 10p13 for a series of neighboring microsatellite markers, providing evidence for a major locus for this prevalent infectious disease. Thus, despite the polygenic nature of infectious disease susceptibility, some major, non-HLA-linked loci exist that may be mapped through obtainable numbers of affected sibling pairs.-Authors' Abstract
Spierings, E., de Boer, T., Wieles, B., Adams, L. B., Marani, E. and Ottenhoff, T. H. Mycobacterium leprae-v.ptcific, HLA Class II-restricted killing of human Schwann cells by CD4+ THI cells: a novel immunopathogenic mechanism of nerve damage in leprosy. J. Immunol. 166(2001)5883-5888.
Peripheral nerve damage is a major complication of reversal (or type 1) reactions in leprosy. The pathogenesis of nerve damage remains largely unresolved, but detailed in situ analyses suggest that type 1 T cells play an important role. Mycobacterium leprae is known to have a remarkable tropism for Schwann cells of the peripheral nerve. Reversal reactions in leprosy are often accompanied by severe and irreversible nerve destruction and are associated with increased cellular immune reactivity against M. leprae. Thus, a likely immunopathogenic mechanism of Schwann cell and nerve damage in leprosy is that infected Schwann cells process and present Ags of M. leprae to Ag-specific, inflammatory type 1 T cells and that these T cells subsequently damage and lyse infected Schwann cells. Thus far it has been difficult to study this directly because of the inability to grow large numbers of human Schwann cells. We now have established long-term human Schwann cell cultures from sural nerves and show that human Schwann cells express MHC class I and II, ICAM-1, and CD80 surface molecules involved in Ag presentation. Human Schwann cells process and present M. leprae, as well as recombinant proteins and peptides to MHC class II-restricted CD4+ T cells, and are efficiently killed by these activated T cells. These findings elucidate a novel mech anism that is likely involved in the immunopathogenesis of nerve damage in leprosy.-Authors' Abstract
Spierings, F., De Boer, T., Zulianello, L., and Ottenhoff, T. H. M. The role of Schwann cells, T cells and Mycobacterium leprae in the immunopathogenesis of nerve damage in leprosy. Lepr. Rev. 71 Suppl.(2000)S121-SI29.
Damage to peripheral nerves is the major complication of reversal (type 1) reactions in leprosy. The underlying mechanism of nerve damage remains largely unresolved; however, an important role for type-1 T cells has been suggested. Mycobacterium leprae has a remarkable tropism for the Schwann cells that surround peripheral axons. Because reversal reactions in leprosy are often accompanied by severe and irreversible nerve destruction, and are associated with increased cellular immune reactivity against M. leprae, a likely immunopathogenic mechanism of damage to Schwann cells and peripheral nerves in leprosy is that infected Schwann cells process and present antigens of M. leprae to antigen-specific, inflammatory, type-1 T cells, and that these T cells subsequently damage and lyse infected Schwann cells. Previous animal studies with CD8+ T cells revealed evidence for the existence of such a mechanism. A similar role has been suggested for CD4+ T cells. These latter cells may be more important in causing nerve damage in vivo, given the predilection of M. leprae for Schwann cells, and the dominant role of CD4+, serine esterase+ Till cells in the lesions of leprosy. Antagonism of the molecular interactions among M. leprae, Schwann cells and inflammatory T cells may therefore provide a rational strategy for prevention of damage of Schwann cell and nerves in leprosy.-Authors' Summary
Tovar-Rivera, T., Sanchez-Colon, S., Padierna-Olivos, L., Masso-Rojas, F., Estrada-Parra, S., Mondragon-Gonzalez, R., Jimenez-Martinez, M. C. and Sanchez-Garcia, F. J. Connectivity patterns in tuberculosis and leprosy patients are indistinguishable from that of healthy donors. Scand. J. Immunol. 53(2001)520-527.
Connectivity, the self-defined interactions between antigen-recognizing molecules in a network system, can in part be assessed by measuring the reactivity of a given serum against an ordered set of immunoglobulin (lg)G F(ab')2 fractions, separated by means of isoelectric focusing so that the serum reactivity against the whole set of fractions defines a characteristic pattern of connectivity. Deviations from the normal condition (healthy donors) have so far been documented for two autoimmune diseases: systemic lupus erythematosus (SLE) and pemphigus vulgaris, as well as for human immunodeficiency virus (HIV)-I infection. We tested here if bacterial infections lead to alterations in connectivity. In addition, we wanted to test if two antigenically related bacteria would produce similar or otherwise distinctive connectivity patterns. Connectivity analysis was applied on the sera from tuberculosis and leprosy patients and the sera from healthy donors were used as control. No statistically significant differences between the three groups studied were found. These results have implications for theories that set the origin of autoimmune diseases in microbial infections. To the best of our knowledge, this is the first attempt to analyze the connectivity status in bacterial infections.-Authors' Abstract
Vemuri, N. Cytokine patterns using molecular tools. Indian J. Lepr. 72(2000)175-185.
The role of CD4+ helper T cells (Th1cells and Tli2-cells) and cytokines in the protective immunity to Mycobacterium leprae infection, and the use of cytokines in immunotherapy and as a diagnostic tool are discussed. The methodologies for assessing cytokine responses are enumerated.-Trop. Dis. Bull. 98(2001)923
MICROBIOLOGY
Brennan, P. J. Skin test development in leprosy: progress with first-generation skin test antigens, and an approach to the second generation. Lepr. Rev. 71 Suppl.(2000)S50-S54.
One of the most urgent needs from leprosy research is a test for infection. The lepromin test is not suitable as a diagnostic test for leprosy, and neither the Rees nor the Convit soluble antigens has appeared sufficiently specific. Because two new antigens, MLSA-LAM and MLCwA, may not fully meet the requirements for specificity, we have embarked upon the preparation of a second generation of skin test antigens. Size-fractionated cryptozoic proteins were prepared from M. leprae by electroelution from preparative sodium dodecylsuphatepolyacrylamide gel electrophoresis, and individual fractions were probed with polyclonal and monoclonal antibody reagents to identify both known and novel proteins. In addition, immunological responses were assessed in M. leprae-sensitized guinea pigs against both crude subcellular fractions (cytosol, membrane, and soluble cell wall proteins) and the size-fractionated cytosolic proteins. A particularly promising subcellular fraction is the membrane fraction of M. leprae, which contains many proteins unique to the organism. Clinical trials of the M. leprae membrane proteins are now being planned.-Author's Summary
Cole, S. T., Eiglmeier, K., Parkhill, J,, James, K. D., Thomson, N. R., Wheeler, P. R., Honore, N., Gamier, T., Churcher, C., Harris, D., Mungall, K., Basham, D., Brown, D., Chillingworth, T., et al. Massive gene decay in the leprosy bacillus. Nature 409(2001)1007-1011.
Leprosy, a chronic human neurological disease, results from infection with the obligate intracellular pathogen Mycobacterium leprae, a close relative of the tubercle bacillus. M. leprae has the longest doubling time of all known bacteria and has thwarted every effort at culture in the laboratory. Comparing the 3.27-megabase (Mb) genome sequence of an armadillo-derived Indian isolate of the leprosy bacillus with that of M. tuberculosis (4.41 Mb) provides clear explanations for these properties and reveals an extreme case of reductive evolution. Less than half of the genome contains functional genes but pseudogenes, with intact counterparts in M. tuberculosis, abound. Genome downsizing and the current mosaic arrangement appear to have resulted from extensive recombination events between dispersed repetitive sequences. Gene deletion and decay have eliminated many important metabolic activities including siderophore production, part of the oxidative and most of the microaerophilic and anaerobic respiratory chains, and numerous catabolic systems and their regulatory circuits.-Authors' Abstract
Dockell, H. M., Brahmbhat, S., Robertson, B. D., Britton, S., Fruth, U., Gebre, N., Hunegnaw, M., Hussain, R., Manadhar, R., Murrillo, L., Pessolani, M. C. V., Roche, P., Salgado, J. L., Sampaio, E., Shahid, F., Thole, J. E. R. and Young, D. B. Diagnostic assays for leprosy based on T-cell epitopes. Lepr. Rev. 71 Suppl.(2000)S55-S59.
To date, only a limited number of antigens have been described as specific for Mycobacterium leprae, and in many cases, homologues have subsequently been shown to exist in mycobacteria such as M. avium and M. intracellulare. A Leprosy Synthetic Peptide Skin Test Initiative was established by the Steering Committee on the Immunology of Mycobacteria of the UNDP/World Bank/WHO Special Programme for Research and Training in Tropical Diseases to investigate the potential of synthetic peptides that encode T-cell epitopes as diagnostic tools, which could be used to develop a skin-test reagent specific for leprosy. Such M. leprae-specific peptides should have unique amino acid sequences, or significant sequence-dissimilar ity from those in other mycobacteria. Synthetic peptides, 15 amino acids long, were synthesized from 33 genes or open reading frames within the M. leprae genome. Tuberculoid leprosy patients from four leprosy-endemic countries, Brazil, Ethiopia, Nepal and Pakistan, were tested as subjects known to have been infected with M. leprae, and to make good T-cell responses to antigens of M. leprae; U.K. blood donors were used as nonexposed or noninfected subjects. Peptides inducing potentially specific responses in leprosy patients and not in U.K. controls, and those inducing crossreaction responses, present in both leprosy patients and nonexposed, noninfected controls, were identified. A difference from the equivalent M. tuberculosis sequence of five or more amino acid residues did not, by itself, identify peptides that were M. lepraespecific, suggesting that many of these peptides may have homologues in environmental mycobacteria. To date, this approach has identified a number of peptides with greater than 90% specificity and l9%-477e sensitivity, which are undergoing further specificity testing. Such peptides would have great potential as T-cell reagents with which to monitor exposure to M. leprae within communities, formulated either as skin-test reagents, or as antigens for tests in vitro.Authors' Summary
Donoghue, H. D., Holton, J. and Spigelman, M. PCR primers that can detect low levels of Mycobacterium leprae DNA. J. Med. Microbiol. 50(2001)177-182.
There are several specific PCR-based methods to detect Mycobacterium leprae DNA, but the amplicons are quite large. For example, primers that target the 36-kDa antigen gene and are in common diagnosticuse yield a 530-bp product. This may be a disadvantage when examining samples in which the DNA is likely to be damaged and fragmented. Therefore, two sets of M. leprae-specific nested primers were designed, based on existing primer pairs which have been shown to be specific for M. leprae. Primers that targeted the 18-kDa antigen gene gave an outer product of 136 bp and inner product of 100 bp. The primers based on the RLEP repetitive sequence yielded a 129-bp outer product and 99-bp nested product. With dilutions of a standard M. leprae killed whole-cell preparation as the source of DNA, both single-stage and nested PCR were performed after optimization of the experimental conditions. Compared with the 36-kDa antigen gene primers, the 18-kDa antigen gene outer primers were 100-fold more sensitive, and the RLEP outer primers were 1000-fold more sensitive. As an illustration of two possible applications of these new primers, positive results were obtained from three slit-skin samples from treated lepromatous leprosy patients and three archaeological samples from human remains showing typical leprosy paleopathology. It was concluded that these new primers are a useful means of detecting M. leprae DNA which is damaged or present at a very low level.Authors' Abstract
Gillis, T. P. and Williams, D. L. Dapsone resistance in Mycobacterium leprae. Lepr. Rev. 71 Suppl.(2000)S91-S95.
The folPI gene of Mycobacterium leprae, which encodes dihydropteroate synthase (DHPS), was studied for the presence of mutations associated with resistance to dapsone (DDS). When the folPI of several DDS-resistant clinical isolates of M. leprae were sequenced, two missense mutations were identified. One mutation occurred at codon 53, substituting isoleucine for threonine in DHPS-1, and a second mutation occurred in codon 55, substituting arginine for proline. DNA sequencing of strains of M. leprae resistant to 0.01 g% DDS in the mouse diet revealed that 13 of 14 strains contained either the 53 or 55 folpi mutation. None of the susceptible strains and only one of five strains resistant to 0.001 g% DDS revealed a mutation in folP\, suggesting that only high-level DDS resistance is associated with the mutations identified in folpi. Development and application of simple molecular tests to assess drug-related mutations in M. leprae could establish current levels of drug resistance in leprosy as a reference point for future monitoring of drug resistance at the global level.-Authors' Summary
Katoch, V. M. and Sharma, V. D. Recent advances in the microbiology of leprosy. Indian J. Lepr. 72(2000)363-379.
The biology (morphology, chemical features, antigenic structure, gene sequences related to physiology, phylogenetics and gene expression in host-vector systems), metabolism, cultivation, persistence and dormancy of Mycobacterium leprae are summarized. Methods for detecting M. leprae, assessing their load and viability, and understanding their molecular epidemiology are discussed. Drugs used to treat leprosy are enumerated and the mechanism of drug resistance is mentioned.-Trop. Dis. Bull 98(2001)1694
Keer, J., Smeulders, M. J. and Williams, H. D. A purF mutant of Mycobacterium smegmatis has impaired survival, during oxygen-starved stationary phase. Microbiology-U.K. 147(2001)473-481.
In this study it was demonstrated that a range of transposon mutants of Mycobacterium smegrnatis, previously described as having impaired survival in carbon-starved stationary phase, were not markedly affected in O2-starved stationary-phase survival. One exception was 329B, a purine auxotroph, which showed a precipitous reduction in viability from similar to 108 to similar to 10-1 c.f.u. ml 1 during the first 5-10 days in O2-starved stationary phase. This was followed by an equally rapid recovery in culturability to a level within 10 to 100-fold of wildtype levels by 10-20 days into the stationary phase. Transduction of the mutation into a clean genetic background demonstrated that the phenotype was due to the transposon insertion, which was shown to be in the purF gene. PurF encodes phosphoribosylpyrophosphate amidotransferase, which catalyzes the first committed step in purine biosynthesis. The M. smegrnatis purF gene, which encodes a protein with a very high degree of similarity to the PurF homologs of M. tuberculosis and M. leprae, was cloned and shown to substantially complement the O2-starvation phenotype. The recovery in culturability of the purF mutant in 0,-starved stationary phase did not involve movement of the transposon. In addition, when cells that had recovered culturability were retested, their survival kinetics in stationary phase were identical to the original culture, indicating that their recovery was not explained by the accumulation of suppressor mutations. It is concluded that the survival curve in O,starved stationary phase for the purF mutant represents its true phenotype and is not a result of subsequent genetic changes in the culture. It is argued that the purF cells lose culturability for a finite period of time in stationary phase. Whether this is due to a fraction of the population dying and then regrowing using a previously undiscovered fermentation pathway, or becoming transiently dormant, or entering an active nonculturable state and subsequently undergoing resuscitation cannot be distinguished at this stage.-Authors' Abstract
Limia, A., Sangari, F. J., Wagner, D. and Bcrmudcz, L. E. Characterization and expression of secA in Mycobacterium avium. FEMS Microbiol. Lett. 197 (2001)151-157.
Mycobacterium avium is both a pathogen that infects several hosts such as humans, pigs, and birds, as well as a microorganism that is encountered in environmental sources (soil and water). Protein secretion by the bacterium is likely to influence its ability to overcome adverse and competitive conditions both within or outside the host. Using a combination of cloning and information available in the databank, we characterized the secA gene from M. avium, encoding for a major preprotein translocase subunit associated with the secretion system of prokaryotics. In addition, we cloned the secA promoter sequence in a reporter construct upstream of a promoterless gfp. It was determined that the secA of M. avium shares large homology with the secA of M. tuberculosis but not with secA of M. leprae. secA expression was determined to be greater at logarithmic growth phase although it was also expressed at low levels during the stationary phase. secA expres sion was also observed when the bacteria were incubated in water as well as within human monocyte-derived macrophages and in conditions that are associated with biofilm formation. Future evaluation of the sec pathway in M. avium might provide important information about secreted proteins that are required for survival in different environments.-Authors' Abstract
Marques, M. A., Mahapatra, S., Sarno, E. N., Santos, S., Spencer, J. S., Brennan, I'. J. and Pessolani, M. C. Further biochemical characterization of Mycobacterium leprae laminin-binding proteins. Braz. J. Med. Biol. Res. 34(2001)463-470.
It has been demonstrated that the alpha2 chain of laminin-2 present on the surface of Schwann cells is involved in the process of attachment of Mycobacterium leprae to these cells. Searching for M. leprae laminin-binding molecules, in a previous study we isolated and characterized the cationic proteins histone-like protein (Hip) and ribosomal proteins S4 and S5 as potential adhesins involved in M. lepraeSchwann cell interaction. Hip was shown to bind alpha2-Iaminins and to greatly enhance the attachment of mycobacteria to ST88-I4 Schwann cells. In the present study, we investigated the laminin-binding capacity of the ribosomal proteins S4 and S5. The genes coding for these proteins were PCR amplified and their recombinant products were shown to bind alpha2laminins in overlay assays. However, when tested in ELISA-based assays and in adhesion assays with ST88-14 cells, in contrast to Hip, S4 and S5 failed to bind laminin and act as adhesins. The laminin-binding property and adhesion capacity of two basic host-derived proteins were also tested, and only histones, but not cytochrome c, were able to increase bacterial attachment to ST88-14 cells. Our data suggest that the alanine/lysine-rich sequences shared by Hip and eukaryotic HI histones might be involved in the binding of these cationic proteins to laminin.-Authors' Abstract
Petite, K., Puech, V., Daffe, M., Josenhans, C., Drobecq, H., Locht, C. and Menozzi, F. D. Mycobacterium smegnuttis laminin-binding glycoprotein shares epitopes with Mycobacterium tuberculosis heparin-binding haemagglutinin. Mol. Microbiol. 39(2001)89-99.
Mycobacterium tuberculosis, the causative agent of tuberculosis, produces a heparinbinding hemagglutinin adhesin (HBHA) which is involved in its epithelial adherence. To ascertain whether HBHA is also present in fast-growing mycobacteria, M. smegmatis was studied using anti-HBHA monoclonal antibodies (mAbs). A crossreactive protein was detected by immunoblotting of M. smegmatis whole-cell lysates. However, the M. tuberculosis HBHA-encoding gene failed to hybridize with M. smegnuitis chromosomal DNA in Southern blot analyses. The M. smegnuitis protein recognized by the anti-HBHA mAbs was purified by heparin-Sepharose chromatography, and its amino-terminal sequence was found to be identical to that of the previously described histone-like protein, indicating that M. smegmatis does not produce HBHA. Biochemical analysis of the M. smegmatis histone-like protein shows that it is glycosylated like HBHA. Immunoelectron microscopy demonstrated that the M. smegmatis protein is present on the mycobacterial surface, a cellular localization inconsistent with a histone-like function, but compatible with an adhesin activity. In vitro protein interaction assays showed that this glycoprotein binds to laminin. a major component of basement membranes. Therefore, the protein was called M. smegmatis laminin-binding protein (MS-LBP). MSLBP does not appear to be involved in adherence in the absence of laminin but is responsible for the laminin-mediated mycobacterial adherence to human pneumocytes and macrophages. Homologous lamininbinding adhesins are also produced by virulent mycobacteria such as M. tuberculosis and M. leprae, suggesting that this adherence mechanism may contribute to the pathogenesis of mycobacterial diseases.Authors' Abstract
Ramasoota, P., Wongwit, W., Sampunachot„ P., Unnarat, K., Ngamying, M. and Svenson, S. B. Multiple mutations in the rpoB gene of Mycobacterium leprae strains from leprosy patients in Thailand. SE Asian J. Trop. Med. Pub. Health 31(2000)493-497.
A new finding is reported of multiple mutations in the rpoB gene of 9 Mycobacterium leprae strains from leprosy patients in Thailand, who did not respond to therapy even when rifampin, the main drug in multidrug therapy was used. By means of sequence analysis of 9 Thai M. leprae strains, various mutations in 289 bps of the rpoB gene revealed forms of mutation never before described, such as multiple mutations (i.e., mutation at 2, 3, 6, 7, 8 and 9 positions in the rpoB gene), most of which were point-mutation substitutions (a few of which were silent), and some insertions. This investigation demonstrates that mutation in the rpoB gene of M. leprae strains from Thailand involves more variety than previously reported for rpoB mutation patterns in rifampin-resistant M. leprae strains.-Authors' Abstract
Rastogi, N., Legrand, E. and Sola, C. The mycobacteria: an introduction to nomenclature and pathogenesis. Rev. Sci. Tech. 20(2001)21-54.
Tuberculosis, caused by Mycobacterium tuberculosis, and leprosy, caused by M. leprae, are diseases known since antiquity. In developing countries, tuberculosis is still the leading cause of mortality due to an infectious disease. Taxonomically, mycobacteria belong to the genus Mycobacterium, which is the single genus within the family of Mycobacteriaceae, in the order Actinomycetales. Actinomycetales include diverse micro-organisms, but mycobacteria and allied taxa are easily distinguished on the basis of the ability to synthesize mycotic acids. Mycobacterial species are traditionally differentiated on the basis of phenotypic characteristics, and the authors provide an updated list of the biochemical tests currently employed and the culture properties that help to discriminate among various species of mycobacteria. However, as the phenotypic characteristics do not allow precise identification of all species, recent molecular taxonomical approaches for mycobacterial classification and phylogeny are also described. Mycobacteria are also a leading cause of infection in various domesticated animals and wildlife. The authors briefly describe the mycobacteria involved in animal infections, the wildlife reservoirs and strategies to control bovine tuberculosis, and the use of molecular tools for diagnostics and epidemiology of mycobacterial infections in animals. The characteristic of intracellular parasitism is discussed. in addition to the fate of pathogenic mycobacteria that have the ability to grow inside phagosomes and phagolysosomes of infected host macrophages. The mycobacterial cell envelope, which is a complex tripartite structure containing a high proportion of lipids (approximately 30% to 40% of the total weight), could play a crucial role in the adaptation of mycobacteria to intracellular growth and survival, immune modulation and drug resistance.-Authors' Abstract
Sengupta, U. Experience and lessons from the use of lepromin and Mycobacterium leprae-spccific serology. Lepr. Rev. 71 Suppl.(2000)S63-S66.
Skin testing with lepromin, which produces a delayed-type hypersensitivity reaction, has been used in the classification of leprosy, and a good correlation has been found between immunological status and the reaction to lepromin. In addition, the prognostic value of the lepromin test has been demonstrated. More recently, skin testing with two soluble antigens of Mycobacterium leprae showed no difference of the mean size of the reaction between household contacts and noncontacts, indicating that these antigens are not useful for the diagnosis of leprosy. This and other evidence points to the need for a better skin test antigen capable of detecting infection of individuals by M. leprae. Whereas serological assays for antibodies against both PGL-I and the 35-kDa antigen of M. leprae have been found to yield positive results in 90%-100% of patients with lepromatous (BL/LL) leprosy, these assays fail to identify 40%-60% of patients with tuberculoid (BT/TT) leprosy, because of the presence of only an insignificant level of antibody against components of M. leprae in these patients' sera, although, in many BT patients, antibody signal could be detected in the local lesions. These data indicate that there remains a need for a specific diagnostic test for leprosy.-Author's Summary
Shin, Y. C., Lee, H., Lee, H., Walsh, G. P., Kim, J. D, and Cho, S. N. Variable numbers of TTC repeats in Mycobacterium leprae DNA from leprosy patients and use in strain differentiation. J. Clin. Microbiol. 38(2000)4535-4538.
Strain differentiation of Mycobacterium leprae would be of great value for epidemiological investigation to identify the infectious sources of leprosy, to understand transmission patterns, and to distinguish between relapse and reinfection. From the M. leprae genome sequence database, TTC DNA repeats were identified. Primer sets designed to amplify the region flanking TTC repeats revealed PCR products of different sizes, indicating that the number of repeats at each locus may be variable among M. leprae strains. The TTC repeats were not found in M. tuberculosis, M. avium, M. marinum, or human tissues, which indicated their specificity to M. leprae. Sequence analysis of the TTC repeat region in each of the M. leprae strains showed a variation of 10 to 37 repeats. In the M. leprae strains of 34 multibacillary patients at Cebu, the Philippines, M. leprae with 24 and 25 1TC repeats was most common, and this was followed by strains with 14, 15, 20, 21, and 28 repeats. This study thus indicates that there are variable numbers of TTC repeats in a noncoding region of M. leprae strains and that the TTC region may be useful for strain differentiation for epidemiological investigations of leprosy.-Authors' Abstract
Sugita, Y. [PCR in leprosy.] Jpn. J. Hansen's Dis. 70(2001)3-13. (in Japanese)
Detection of M. leprae DNA using PCR is very sensitive, enough to detect very few numbers of bacilli which are not recognized by the acid-fast staining method. Because the detection of M. leprae is crucial for the diagnosis of leprosy, PCR method has been expected to make a diagnosis easy and precise. A new pair of PCR primers for M. leprae was selected in the Department of Dermatology, Yokohama City University School of Medicine (Japan], and many samples obtained from many institutes have been examined in the department. In this paper, the PCR method in leprosy is discussed, and the results of examination of 59 cases carried out in the department from 1994 until 2000 are demonstrated.-Author's English Abstract
EPIDEMIOLOGY AND PREVENTION
Ashford, D. A,, Whitney, E., Raghunathan, F. and Cosivi, O. Epidemiology of selected mycobacteria that infect humans and other animals. Rev. Sci. Tech. 20(2001)325-327.
This paper provides a summary of salient clinical and epidemiological features of selected mycobacterial diseases that are common to humans and other animals. Clinical and diagnostic issues are discussed and related to estimates of the incidence and prevalence of these diseases among humans. Source of infection, route of transmission and control measures are also presented. The mycobacteria discussed in this paper are Mycobacterium bovis, M. ulcerans, M. leprae and M. avium complex, although this is by no means a complete list of the mycobacteria common to humans and other animals. Certain generalities can be made regarding these species of mycobacteria and their occurrence in humans and other animals; firstly, current understanding of the epidemiology and control of many of the resultant diseases is incomplete; secondly, environmental sources other than animal reservoirs may play a role in transmission (with M. leprae perhaps being the exception); and thirdly, the incidence and prevalence of these diseases in many countries of the world are unclear, principally because of the complexity of diagnosis and lack of reporting systems.-Authors' Abstract
Chen, X.-S., Li, VV.-Z., Jiang, C. and Ye, G.-Y. Leprosy in China: epidemiological trends between 1949 and 1998. Bull. WHO 79(2001)306-312.
Objective: To report the epidemiological trends of leprosy in China from 1949 to 1998. Method: Data for the study were obtained from the computerized database of the National System of Leprosy Surveillance. Findings: A total of 474,774 leprosy patients were detected during this 50-year period. Case detection rates per 100,000 population were highest in the 1950s and 1960s, with peaks appearing 1957-1958, 1963-1966, 1969-1970, and 1983-1984, corresponding to mass surveys or screening surveys carried out in most areas or selected areas of the country. While the duration of the disease at the time of detection fell over the period, the disability rates, which were >50% in the early 1950s, have decreased gradually to 20.8% by 1997-1998 but are still too high. More than 50% of cases were found through active methods in the periods 1955-1958, 1965-1966, and 1969-1976, but in recent years cases are mostly detected through dermatological clinics or by voluntary reporting. The peak prevalences of the 1960s (i.e., >2 per 10,000 population) decreased annually from the 1970s onward. By the end of 1998 the prevalence was 0.05 per 10,000 population. Conclusions: This study shows that leprosy was well controlled in China and that the WHO goal of elimination of leprosy as a public health problem has been achieved at the national and subnational levels. However, leprosy is still unevenly distributed in the country. According to the criterion for leprosy elimination in China-defined as a prevalence of <1 per 100,000 in county or city-there are still more than 10% of counties or cities where this target has not yet been reached. Special attention must therefore be given to achieve elimination and final eradication of leprosy in China.-Authors' Abstract
Gupta, V., Kumar, B., Rai, R., Kaur, I. and Vasudeva, U. Community based leprosy survey in U.T. Chandigarh. Indian J. Lepr. 72 (2000) 249-251.
A population of 350,000 individuals was scanned for leprosy during 16-21 April 1998 in Chandigarh, India, to search for hidden cases. Of 350,000 individuals, search teams were able to identify 112 confirmed cases of leprosy; 72 of 112 cases reported for follow up but the diagnosis of leprosy was doubtful in 5 of them and they were advised to come for regular follow up. The remaining 67 cases (42 were multibacillary and 25 were paucibacillary cases) were all put on treatment and have successfully completed their treatment. It is concluded that the problem of leprosy in Chandigarh is mostly due to the migrant population that keeps moving in and out of the city and that it is likely to remain high until leprosy is eliminated from the neighboring hisihly endemic states of the country.-Trop. Dis. Bull. 98(2001)928
Haider (Biswas), A., Mundle, M., Bhadra, U. K. and Saha, B. Role of paucibacillary leprosy in the transmission of disease. Indian J. Lepr. 73(2001)11-15.
The objective of this study was to establish that paucibacillary (PB) leprosy also carried increased risk of infection to the community. All members of 100 families with an index PB case were clinically, bacteriologically and immunologically examined. The "comparison" group was sampled from suspect register. Fifty-six cases occurred among 944 contacts of index PB cases; of these, four were multibacillary (MB) and 52 were PB. In the "comparison" group, two contacts out of 760 developed PB leprosy. This difference between the two groups was statistically significant. All 56 cases in the index case families were under 20 years of age and 50 of them were aged under 15 years. Male/female ratio was 2.1:1. Of the 56 cases, 28 shared the same bed with the index patient, 20 shared the same room, and 8 lived in the same house. Lepromin positivity rate was higher in "comparison" families (92.2%) than in index case families (74.6%), the difference being statistically significant (x = 6.09, p <0.001). Contacts of index case families, therefore, were immunologically at higher risk than contacts of "comparison" families.-Authors' Abstract
Inirida Guerreo, M., Plazas, N. and Ines Leon, C. [ Present situation of leprosy in Colombia: a critical analysis.] Biomedica 20(2000)271. (in Spanish)
The current leprosy situation in Colombia is discussed, including disease prevalence, therapy and control programs.Trop. Dis. Bull. 98(2001)943
Keita, S., Tiendrebeogo, A., Konare, H., Cisse, B. S. and Faye, O. New cases of leprosy at the Marchoux Institute: a comparative study 1988-1997. Ann. Dermatol. Venereol. 128(2001)217-219.
Background: The prevalence of leprosy had declined greatly over the last decade. The purpose of this work was to determine whether changes in the epidemiology, clinical and bacteriological patterns occurred among patients with leprosy treated at the Marchoux Institute in 1988 and in 1997. Patients and Methods: We conducted a descriptive cross-sectional study, reviewing retrospectively all files of patients with leprosy seen in 1988 in comparison with a prospective series of leprosy patients seen in 1997. Only new cases of leprosy, prior to treatment and with skin and/or nervous lesions irrespective of the bacilloscopy results, were included in the two series. Results: We included 93 patients among 246 patient files in 1988. There were 119 new cases in 1997. The following variables showed changes: mean delay to consultation (41.2 months in 1988 vs 26.1 months in 1997; patient's suspicion of having leprosy (93 patients in 1988 vs 22 in 1997); notion of contact (35 cases in 1988 vs 45 in 1997). Multibacillary leprosy predominated over paucibacillary leprosy in 1988 (51 vs 42 cases). This trend was inverted in 1997 (44 vs 75) (p <0.009). Patients with grade 2 handicap were more numerous in 1988 (20 cases vs 2 cases, p <0.001). Conclusion: These findings demonstrate a change in the epidemiology, clinical and bacilloscopic pattern of patients with leprosy from 1988 to 1997.-Authors' Abstract
Lana, F. C. F., de Lima, R. F., Araujo, M. G. and Fonseca, P. T. S. [ Epidemiological status of leprosy in the city of Belo Horizonte, Minas Gerais State (Brazil), 1992-1997.] Hansen. Int. 25(2000)121-132. (in Portuguese)
The authors studied the endemic status of leprosy at Belo Horizonte City, Minas Gerais, Brazil. Operational and epidemiological coefficients had been focused. Data on 1217 cases were obtained between 1992-1997 from the leprosy notification bulletin of the Health Division of Minas Gerais State. The detection rates were high for the years 1992-1994, and mild between 1995-1997. The detection of paucibacillary cases was low (15.6%), including indeterminate cases (3.9%). The multibacillary cases observed were 84.4%. Cases diagnosed in children (0-14 years) were 5.6% of the total number, and only 39.7% of patients referred to symptoms less than 12 months prior to diagnosis. The high physical disabilities index observed (10.6%) and the above-cited parameters suggest a delay in the leprosy diagnosis. In this way the possibility of a hidden prevalence is of interest. because it can compromise the goal of leprosy elimination.-Authors' English Summary
Lechat, M. F. The source of infection: an unsolved issue. Indian J. Lepr. 72(2000)169-173.
A paper summarizing the status of case detection and treatment program of Mycobacterium leprae infection is presented. Reasons behind the persistence of the high detection rate of M. leprae infection are discussed.-Trop. Dis. Bull. 98(2001)922
Mandul, B. C. Present leprosy situation in India and the decade long experience of this correspondent. Jpn. J. Hansen's Dis. 70(2001)25-29.
Leprosy, which was known to ancient India as "Kustha Roga," is thought to have its origin from India also. It is still a major public health problem in India, affecting many people every year. India is now having maximum numbers of leprosy cases worldwide and accounts for 67% of total prevalence and 73% of total new case detection. Huge numbers of new cases have been detected in recent years (last year's new cases were 782,501) because of adoption of new strategy, Modified Leprosy Elimination Campaign (MLEC), and effective health education campaign. Presently, 70% of the total new caseloads of India are from the five most heavily infected states. There is significant improvement in the overall situation as is evident from a steady decline of the prevalence rate from 38.6 cases per 10,000 population in 1985 to 5.0 per 10,000 in 1999.-Author's Abstract
Silva, E. A., Rubio, E. M. and Ura, S. [Lewis blood group system in leprosy patients.] Hansen. Int. 25(2000)115-120. (in Portuguese)
The distribution of Lewis blood group phenotypes in the saliva and on the erythrocytes of leprosy patients were evaluated. Forty-seven patients and forty controls were analyzed by means of an agglutination and agglutination inhibition test for the presence of ABH and Lewis antigens on erythrocytes and in the saliva. The frequency of the Lewis phenotypes and secretor and nonsecretor phenotypes were determined among the patients and in the control group. The results were: Le(ab+) = 29.8% (62.5%); Le(a+ b) = 25.5% (7.5%); Le(ab) = 44.7% (30.0%); secretor = 59.5% (85%) and nonsecretor = 40.5% (15%), respectively. Statistical analysis using the χ2 test showed significant difference between patients and controls concerning the Lewis phenotype (%2 = 10.46; DF = 2; p = 0.005) and secretor phenotype (x2 = 5.64; DF = 1; p = 0.018). Using the Z test significant differences were found concerning the phenotypes Le (a+ b) and Le (ab+) (Z = 2.219; p = 0.027 and Z = 3.058; p = 0.002). The results indicate that phenotype Le (a+ b) is associated with susceptibility to leprosy and secretor phenotype with protection. It is speculated that the presence of Leb in the saliva inhibits the adherence of M. leprae to the mucosa cells thus protecting against infection.-Authors' English Summary
World Health Organization. Leprosy global situation. Wkly. Epidemiol. Rec. 75(2000)226-231.
As of I January 2000 in 91 reporting countries, 641,091 leprosy cases were registered for treatment and 678,758 cases were newly detected; the prevalence rate at the global level was around 1.25 per 10,000 population. There were 24 countries where leprosy remained a public health problem and in the top 11 endemic countries the prevalence rate was still 4.1 per 10,000 population. There was a reduction of around 8% in the number of registered cases and a decrease of around 8% in the number of new cases detected between 1998 and 1999. India represented 67% of the prevalence and 73% of the leprosy detection worldwide.-Trop. Dis. Bull. 98(2001)909
Wu, X.-S., Ning, Y., Shi, L., Jin, Z. and Yang, J.-W. An epidemiological analysis of leprosy from 1951-1996 in Sichuan. Indian J. Lepr. 72(2000)215-226.
Through the leprosy surveillance system established in the 1990s, the authors analyzed the epidemiology of leprosy in Sichuan province in China from 19511996. By the end of 1996, the total number of registered cases was 32,772; the peak incidence rate (2.44/100,000) was in 1958. The annual average progressively decreasing speed (AAPDS) of the number of new cases, incidence rate, incidence rate among children, number of newly detected patients, detection rate, number of registered cases and registered prevalence rates were: 4.7% (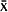 g = 0.9534), 5.9% (
g = 0.9534), 5.9% (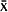 g = 0.9407), 7.4% (
g = 0.9407), 7.4% (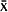 g = 0.9263), 6.7% (
g = 0.9263), 6.7% (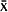 g = 0.9326), 8.1% (
g = 0.9326), 8.1% (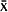 g = 0.9195), 10.9% (
g = 0.9195), 10.9% (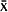 g = 0.8913) and 11.7% (
g = 0.8913) and 11.7% (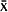 g = 0.8828). respectively. Among newly detected cases, the proportion of children gradually declined with an AAPDS of 2.9% (
g = 0.8828). respectively. Among newly detected cases, the proportion of children gradually declined with an AAPDS of 2.9% (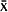 g = 0.9712), but that of household contacts gradually increased, showing a gradual decline of source of infection. The multibacillary (MB) rate among new cases, newly registered cases and active cases also increased gradually. The MB rate among child cases was much lower than that among adults. The disability rates among newly registered cases tended to decline. The peak incidence was in the 20-35-year age group, the average age at onset being 31.92 years. Average age at onset gradually increased to 34.19 during 1991-1995. The average interval between onset of symptoms and diagnosis was 4.89 years and that had reduced gradually to 3.24 years during 1991-1995. The authors conclude that: 1) the epidemiological trend of leprosy in Sichuan province shows decline; 2) the case-finding activities have improved and intensified; but 3) the disability rate among newly detected cases is still high (>20%) and the average delay in diagnosis is still too long, showing that early case finding is still not satisfactory.-Trop. Dis. Bull. 98(2001)926
g = 0.9712), but that of household contacts gradually increased, showing a gradual decline of source of infection. The multibacillary (MB) rate among new cases, newly registered cases and active cases also increased gradually. The MB rate among child cases was much lower than that among adults. The disability rates among newly registered cases tended to decline. The peak incidence was in the 20-35-year age group, the average age at onset being 31.92 years. Average age at onset gradually increased to 34.19 during 1991-1995. The average interval between onset of symptoms and diagnosis was 4.89 years and that had reduced gradually to 3.24 years during 1991-1995. The authors conclude that: 1) the epidemiological trend of leprosy in Sichuan province shows decline; 2) the case-finding activities have improved and intensified; but 3) the disability rate among newly detected cases is still high (>20%) and the average delay in diagnosis is still too long, showing that early case finding is still not satisfactory.-Trop. Dis. Bull. 98(2001)926
REHABILITATION
Dong, L.-YV., Li, F.-T., Jiang, J.-A. and Zhang, G.-C. Techniques for covering soft tissue defects resulting from plantar ulcers in leprosy: Part V. Use of the flap in the inguinal region and latissimus dorsi musculocutaneous flap. Indian J. Lepr. 72(2000)227-244.
The area of distribution of the superficial circumflex iliac, superficial epigastric and superficial external pudental arteries is large and flaps based on them can meet the requirement of different recipient sites. We have transplanted free flaps based on the superficial epigastric artery for repairing plantar soft tissue defects in 6 leprosy patients [China, date not given.) During the followup examination 58-118 months later there has been no recurrence of ulceration in any of these cases. The latissimus dorsi muscle is mainly nourished by the thoracodorsal artery and the latissimus dorsi musculocutaneous flap is a large sized, composite structure with abundant blood provision and strong anti-infectious property. The latissimus dorsi flap can be used as an artery pedicled island flap or as a free flap in addition to its use as a muscle graft because of its constant vascular position, wide outer diameter of the vessels and long pedicle. It can therefore be utilized for repairing soft tissue defect or replacement of paralyzed muscle. We have used the latissimus dorsi musculocutaneous free flap for repairing large skin and soft tissue defects resulting from plantar ulceration in 3 leprosy patients. During the follow-up period, one patient who had complete drop-foot and had refused corrective surgery had recurrence of the ulcer in the 12th postoperative month. No ulcers had recurred in the other 2 cases during the follow-up at 48 and 114 months.-Trop. Dis. Bull. 98(2001)927
Kathe, V. J. and Naik, S. S. Leprosy patients and their spouses. Indian J. Lepr. 72(2000)248-249.
One hundred sixteen leprosy patients (60 women and 56 men, aged 30-55 years) attending outpatient clinics in Mumbai, India [date not given] and their healthy spouses were interviewed to determine their views regarding the impact of diagnosis of leprosy and its treatment on their family relationship; 46 women (77%) said that their husbands were cooperative and that they were having a normal marital life. The other 14 women (23%) had trouble in the family initially when the diagnosis was disclosed but that settled down when the treatment progressed. Fifty-one women (85%) had started their treatment within 2 weeks of diagnosis with no financial loss because most of them were housewives and 56 (94%) were cured with the treatment. All of them did not hide their disease from their hushands. A 97% acceptance of female leprosy patients by their healthy spouses was found. Of 56 male patients, 41 (73%) said that their wives were cooperative and had a normal marital life. The other 15 patients (27%) had problem in the family initially after the diagnosis but it subsided as the treatment progressed; 53 patients (95%) started their treatment within 2 weeks of diagnosis. Nine of them (16%) suffered financial loss. Most patients accepted the diagnosis and were happy with the treatment; 55 (98%) did not hide their disease from their wives; 95% of male leprosy patients were accepted by their wives.-Trop. Dis. Bull. 98(2001)931
Srinivasan, H. Disability and rehabilitation in leprosy: issues and challenges. Indian J. Lepr. 72(2000)317-337.
The prevalence, risk and severity of impairments due to leprosy are reviewed. A summary of the changes in impairment status during and after multiple drug therapy are tabulated. Some of the consequences of leprosy, such as mortality rate and social isolation, are discussed. Some of the issues involved and their relevance to the programs for disability management and rehabilitation are included.-Trop. Dis. Bull. 98(2001)1691
OTHER MYCOBACTERIAL DISEASES AND RELATED ENTITIES
Boechat, N., Bouchonnet, F., Bonay, M., Grodet, A., Pelicic, V., Gicquel, B. and Hance, A. J. Culture at high density improves the ability of human macrophages to control mycobacterial growth. J. Immunol. 166(2001)6203-6211.
The mechanisms through which granuloma formation helps control mycobacterial infection are poorly understood, but it is possible that the accumulation of 'macrophages at high density at sites of infection promotes the differentiation of macrophages into cells with improved mycobactericidal activity. To test this possibility, varying numbers of monocytes were cultured in 96-well plates for 3 days, infected with Mycobacterium bovis bacillus Calmette-Guerin, and the mycobacterial number was assessed 7 days after infection based on the measurement of luciferase activity expressed by a mycobacterial reporter strain or by counting CFU. Mycobacterial growth was optimal in cultures containing 5 x 104 cells/well, but increasing the number of cells to 2 x 105 cells/well resulted in complete inhibition of mycobacterial growth. This effect could not be explained by differences in mycobacterial uptake, multiplicity of infection, acidification of the extracellular medium in high density cultures, enhanced NO production, or paracrine stimulation resulting from secretion of cytokines or other proteins. The morphology of cells cultured at high density was strikingly different from that of monocytes cultured at 5 x 104 cells/well, including the appearance of numerous giant cells. The bacteriostatic activity of monocyte-derived macrophages was also dependent on cell number, but fewer of these more mature cells were required to control mycobacterial growth. Thus, the ability of human macrophages to control mycobacterial infection in vitro is influenced by the density of cells present, findings that may help explain why the formation of granulomas in vivo appears to be a key event in the control of mycobacterial infections.-Authors' Abstract
Chitale, S., Ehrt, S., Kawamura, I., Fujimura, T., Shimono, N., Anand, N., Lu, S., Cohen-Gould, L. and Riley, L. W. Recombinant Mycobacterium tuberculosis protein associated with mammalian cell entry. Cell Microbiol. 3(2001)247-254.
The ability to gain entry and resist the antimicrobial intracellular environment of mammalian cells is an essential virulence property of Mycobacterium tuberculosis. A purified recombinant protein expressed by a 1362 bp locus (niceI) in the M. tuberculosis genome promoted uptake into HeLa cells of polystyrene latex microspheres coated with the protein. N-terminus deletion constructs of Mcel identified a domain located between amino acid positions 106 and 163 that was needed for this cell uptake activity. Mcel contained hydrophobic stretches at the N-terminus predictive of a signal sequence, and colloidal gold immunoelectron microscopy indicated that the corresponding native protein is expressed on the surface of the M. tuberculosis organism. The complete M. tuberculosis genome sequence revealed that it contained four homologues of nice (mcel, mce2. mce3, mce4) and that they were all located within operons composed of genes arranged similarly at different locations in the chromosome. Recombinant Mce2, which had the highest level of identity (67%) to Mcel, was unable to promote the association of microspheres with HeLa cells. Although the exact function of Mcel is still unknown, it appears to serve as an effector molecule expressed on the surface of M. tuberculosis that is capable of eliciting plasma membrane perturbations in non-phagocytic mammalian cells.-Authors' Abstract
Domenech, P., Barry, C. E. and Cole, S. T. Mycobacterium tuberculosis in the post-genomic age. Cuit. Opin. Microbiol. 4(2001)28-34.
Since the publication of the complete genome sequence of Mycobacterium tuberculosis in 1998, there has been a marked intensification and diversification of activities in the field of tuberculosis research. Among the areas that have advanced spectacularly are comparative genomics, functional genomics-notably the study of the transcriptome and proteome-and cell envelope biogenesis, especially as it relates to the mechanism of action of antimycobacterial drugs.-Authors' Abstract
Gomez, A., Mve-Obiang, A., Vray, B., Rudnicka, W., Shaniputa, I. C., Portaels, F., Meyers, W. M., Fonteyne, P. A. and Realini, L. Detection of phospholipase e in nontuberculous mycobacteria and its possible role in hemolytic activity. J. Clin. Microbiol. 39(2001)1396-1401.
Phospholipase C plays a key role in the pathogenesis of several bacterial infections, for example, those caused by Clostridium perfringens and Listeria monocytogenes. Previous studies have reported multiple copies of pic genes homologous to Pseitdomonas aeruginosa plcH and pIcN genes encoding the hemolytic and nonhemoltyic phospholipase C enzymes in the genomes of Mycobacterium tuberculosis. M. marinum, M. bovis, and M. ulcerans. In this study we analyzed the possible relationship between phospholipase C and hemolytic activity in 21 strains of nontuberculous mycobacteria representing 9 different species. Detection of phospholipase C enzymatic activity was carried out using thinlayer chromatography to detect diglycerides in the hydrolysates of radiolabeled phosphatidylcholine. DNA sequences of M. kansasii and M. marinum homologous to the genes encoding phospholipase C from M. tuberculosis and M. ulcerans were identified by DNA-DNA hybridization and sequencing. Finally, we developed a direct and simple assay to detect mycobacterial hemolytic activity. This assay is based on a modified blood agar medium that allows the growth and expression of hemolysis of slow-growing mycobacteria. Hemolytic activity was detected in M. avium. M. intracellulare, M. ulcerans, M. marinum, M. tuberculosis, and M. kansasii with phospholipase C activity, but not in M. fortuitum. No hemolytic activity was detected in M. smegmatis, M. gordonae, and M. vacate. Whether or not phospholipase C enzyme plays a role in the pathogenesis of nontuberculous mycobacterial diseases needs further investigation.-Authors' Abstract
Gooding, T. M., Johnson, P. D. R., Campbell, D. E., Hayman, J. A., Hartland, E. L., Kemp, A. S. and Robins Browne, R. M. Immune response to infection with Mycobacterium ulcerans. Infect. Immun. 69(2001)1704-1707.
Mycobacterium ulcerans is a slow-growing, acid-fast bacillus that causes chronic necrotizing skin ulcers known as Buruli ulcers. Previously reported information on immunity to this mycobacterium is limited. We examined immune responses to M. ulcerans and M. bovis BCG in patients with M. ulcerans and in 20 healthy control subjects (10 tuberculin-test positive and 10 tuberculin-test negative). Cell-mediated immunity was assessed by stimulating peripheral blood mononuclear cells (PBMC) with whole mycobacteria and then measuring PBMC proliferation and the production of gamma interferon (IFN-γ). Humoral immunity was assessed by immunoblotting. PBMC from all subjects showed significantly greater proliferation and IFN-γ production in response to stimulation with living mycobacteria compared with killed cells. However, PBMC from subjects with past or current M. ulcerans disease showed significantly reduced proliferation and production of IFN-γ in response to stimulation, with live M. ulcerans or M. bovis than PBMC from healthy, tuberculin test-positive subjects (p <0.001) and showed results in these assays comparable to those of tuberculin test-negative subjects (p >0.2). Serum from 9 of 11 patients with M. ulcerans disease, but no control subject, contained antibodies to M. ulcerans. The results indicate that patients with M. ulcerans infection mount an immune response to M. ulcerans as evidenced by antibody production, but they demonstrate profound systemic T-cell anergy to mycobacterial antigens. These findings may explain some of the distinct clinical and pathological features of M. ulcerans mduced disease.-Authors' Abstract
Hamasur, B., Burchfeld, J., Haile, M., Pawlowski, A., Bjorvatn, B., Kallenius, G. and Svenson, S. B. Rapid diagnosis of tuberculosis by detection of mycobacterial lipoarabinomannan in urine. J. Microbiol. Methods 45(2001)41-52.
There is an urgent need for improved tools for laboratory diagnosis of active tuberculosis (TB). Here, we describe two methods: a catch-up ELISA and a dipstick test based on the detection in urine of lipoarabinomannan (LAM). LAM is a major and specific glycolipid component of the outer mycobacterial cell wall. Preliminary experiments showed that LAM is excreted in the urine of mice injected intraperitoneally with a crude cell wall preparation of Mycobacterium tuberculosis. Both methods were highly sensitive, detecting LAM at concentrations of I ng/ml and 5 pg/ml, respectively. Of 15 patients with active TB, all showed intermediate to high levels of LAM in their urine (absorbance values from 0.3 to 1.2, mean 0.74). Only one sample showed an absorbance value below the chosen cut-off value of 0.4. All but one of the urine samples from 26 healthy nursing workers exhibited OD value below the 0.4 cut off. These methods may prove valuable for rapid and simple diagnosis of TB, in particular in developing countries lacking biosafety level 3 (BSL3) facilities.-Authors' Abstract
Hirsch, C. S., Toossi, Z., Johnson, J. L., Luzze, H., Ntambi, L., Peters, P., McHugh, M., Okwera, A., Joloba, M., Mugyenyi, P., Mugerwa, R. I)., Terebuh, P. and Ellner, J. J. Augmentation of apoptosis and interferon-gamma production at sites of active Mycobacterium tuberculosis infection in human tuberculosis. J. Infect. Dis. 183(2001)779-788.
Pleural tuberculosis (TB) was employed as a model to study T-cell apoptosis at sites of active Mycobacterium tuberculosis (MTB) infection in human immunodeficiency virus (HlV)-coinfected (HIV/TB) patients and patients infected with TB alone. Apoptosis in blood and in pleural fluid mononuclear cells and cytokine immunoreactivities in plasma and in pleural fluid were evaluated. T cells were expanded at the site of MTB infection, irrespective of HIV status. Apoptosis of CD4 and nonCD4 T cells in the pleural space occurred in both HIV/TB and TB. Interferon-gamma (IFN-γ) levels were increased in pleural fluid, compared with plasma. Spontaneous apoptosis correlated with specific loss of MTB-reactive, IFN-γ-producing pleural T cells. Immunoreactivities of molecules potentially involved in apoptosis, such as tumor necrosis factor-alpha, Fas-ligand, and Fas, were increased in pleural fluid, compared with plasma. These data suggest that continued exposure of immunoreactive cells to MTB at sites of infection may initiate a vicious cycle in which immune activation and loss of antigen-responsive T cells occur concomitantly, thus favoring persistence of MTB infection.-Authors' Abstract
Howard, S. T. and Byrd, T. F. The rapidly growing mycobacteria: saprophytes and parasites. Microbes Infect. 2(2000)1845-1853.
Rapidly growing mycobacteria are widespread saprophytes, but approximately onethird of identified species are also opportunistic pathogens in humans and animals, associated with skin, soft tissue, bone, and pulmonary infections as well as disseminated disease. Clinical and experimental evidence indicates a major role for the cellmediated immune response in the pathogenesis of infection.-Authors' Abstract
Kato-Maeda, M., and Small, P. M. User's guide to tuberculosis resources on the Internet. Clin. Infect. Dis. 32(2001)1580-1588.
The World Wide Web has become a source of information for clinicians and researchers about virtually every aspect of tuberculosis (TB). We provide information about TB-related Internet portal sites. We classify selected TB-related Web pages according to user needs. The questions that we address are as follows: (1) Where can 1 find scientific information about TB? (2) Where can I find epidemiologic data? (3) Where can I find literature for laypeople? (4) Where can I find recommendations, guidelines, and clinical decision-making algorithms for management of TB? (5) Where can I find research databases? (6) Where can I find research groups? (7) Where can I find resources for research, teaching, and training? (8) Where can I find information about regulatory action? The total number of TB-related Web pages is immense, their scope is vast, and their content is perpetually changing. Nonetheless, the sites identified here provide the reader with a manageable number of entry points to this increasingly important resource.Authors' Abstract
King, R. D., Karwath, A., Clare, A. and Dehaspe, L. Accurate prediction of protein functional class from sequence in the Mycobacterium tuberculosis and Escherichia coli genomes using data mining. Yeast 17(2000)283-293.
The analysis of genomics data needs to become as automated as its generation. Here we present a novel data-mining approach to predicting protein functional class from sequence. This method is based on a combination of inductive logic programming clustering and rule learning. We demonstrate the effectiveness of this approach on the M. tuberculosis and E. coli genomes, and identify biologically interpretable rules which predict protein functional class from information only available from the sequence. These rules predict 65% of the ORFs with no assigned function in M. tuberculosis and 24% of those in E. coli, with an estimated accuracy of 60%-80% (depending on the level of functional assignment). The rules are founded on a combination of detection of remote homology, convergent evolution and horizontal gene transfer. We identify rules that predict protein functional class even in the absence of detectable sequence or structural homology. These rules give insight into the evolutionary history of M. tuberculosis and E. coli. Authors' Abstract
Koga, T., Kubota, Y., Kiryu, H., Nakayama, J., Matsuzoe, D, and Shirakusa, T. Erythema induratum in a patient with active tuberculosis of the axillary lymph node: IFN-gamma release of specific T cells. Eur. J. Dermatol. 11(2001)48-49.
A 57-year-old woman with tender nodular lesions on her legs, arms, buttocks, and face is reported as a case of erythema induratum (EI) with active tuberculosis of axillary lymph nodes. Both skin nodular lesions and lymph nodes responded positively to antituberculous therapy, the patient's peripheral blood mononuclear cells showed a high proliferation and produced interferon-gamma (IFN-γ) in response to purified protein derivative (PPD). These finding indicate the possibility that PPD-specific T cclls, capable of producing IFN-γ, are likely to be involved in the formation of El as a type of delayed-type hypersensitivity response to mycobacterial antigens at the site of skin lesions.-Authors' Abstract
Malin, A. S., Huygen, K., Content, J., Mackett, M., Brandt, L., Andersen, P., Smith, S. M. and Dockrell, H. M. Vaccinia expression of Mycobacterium tuberculosis-secreted proteins: tissue plasminogen activator signal sequence enhances expression and immunogenicity of M. tuberculosis Ag85. Microbes Infect. 2(2000)1677-1685.
There is increasing evidence to implicate a role for CD8+ T cells in protective immunity against tuberculosis. Recombinant vaccinia (rVV) expressing Mycobacterium tuberculosis (MTB) proteins can be used both as tools to dissect CD8+ T-cell responses and, in attenuated form, as candidate vaccines capable of inducing a balanced CD4+/CD8+ T-cell response. A panel of rVV was constructed to express four immunodominant secreted proteins of MTB: 85A, 85B and 85C and ESAT-6. A parallel group of rVV was constructed to include the heterologous eukaryotic tissue plasminogen activator (tPA) signal sequence to assess if this would enhance expression and immunogenicity. Clear expression was obtained for 85A, 85B and ESAT-6, and the addition of tPA resulted in N-glycosylation and a 4 to 10-fold increase in expression. Female C57BL/6 mice were immunized using the rVV-Ag85 constructs, and interleukin-2 and gamma-interferon were assayed using a co-culture of immune splenocytes and recall antigen. There was a marked increase in cytokine production in mice immunized with the tPA-containing constructs. We report the first data demonstrating enhanced immunogenicity of rVV using a tPA signal sequence, which has significant implications for future vaccine design.-Authors' Abstract
Mogues, T., Goodrich, M. E., Ryan, L., LaCourse, R. and North, R. J. The relative importance of T cell subsets in immunity and immunopathology of airborne Mycobacterium tuberculosis infection in mice. J. Exp. Med. 193(2001)271-280.
Wild-type (WT) and targeted-mutant mice incapable of making alpha beta T cells, gamma delta T cells, class I major histocompatibility complex (MHC), class II MCH, interferon gamma (INF-y) or inducible nitric oxide synthase (NOS2), were infected with Mycobacterium tuberculosis (Mtb) by aerosol, and monitored over time for their ability to a) control infection, b) develop histopathology at sites of infection, and c) survive. WT mice acquired the ability to control and to hold infection at a stationary level from day 20 on. This was associated with the development of a macrophage-dominated alveolitis at sites of infection, with increased synthesis of IFN-γ and NOS2 mRNA. And with a median survival time (MST) of 258.5 days. In the absence of alpha beta T cells. Mtb grew progressively and rapidly to induce a necrotic, neutrophil-dominated lung pathology that killed mice with a MST of 48 days. In the absence of CD4-mediated immunity (class II -/- mice), progressive bacterial growth continued in the lungs and in other organs beyond day 20, resulting in a MST of 77 days. By contrast, in the absence of CD8 T cell-mediated immunity, lung infection was controlled at a I log higher stationary level that induced a similar histopathologic response to that of WT mice, and resulted in a MST of 232 days-Authors' Abstract
Moran, A. J., Treit, J. D., Whitney, J. L., Abomoelak, B., Houghton, R., Skelky, Y. A., Pedral Sampaio, D., Badaro, R. and Nano, F. E. Assessment of the sérodiagnostic potential of nine novel proteins from Mycobacterium tuberculosis. FEMS Microbiol. Lett. 198(2001)31-36.
To identify antigens that would improve the accuracy of serological diagnosis of active tuberculosis, we cloned the genes encoding nine potentially immunogenic secreted or surface-associated proteins of Mycobacterium tuberculosis. Recombinant proteins were reacted with sera from HIVnegative individuals with extrapulmonary tuberculosis (EP-TB) or HIV-positive individuals with pulmonary tuberculosis (TBH). Specific and high-level antibody responses were obtained for four recombinant proteins, of which antigen GST-822 was recognized by 60% of EP-TB and 42% of TBH and antigen MBP-506 was recognized by 45% of EP-TB and 61% of TBH. These results suggest that these proteins are strong candidates as subunits in a polyvalent serodiagnostic test.-Authors' Abstract
N'Guessan, K., Kouassi, Y., Bouzid, S., Ehuie, P., Koffi, K., Oniangue, C., Aka, N. and Dosso, M. [Interest and limits of exudate microscopy in Mycobacterium ulcerans infection in Cote d'Ivoire.] Bull. Soc. Pathol. Exot. 94(2001)9-10. (in French)
The objective of this study was to estimate the interest and the limits of skin exudate microscopy for patients with chronic ulceration with clinically suspected Buruli's ulcer and living in an endemic area in Cote d' Ivoire. Two stained smears, one with Ziehl-Neelsen and the other Dugomier staining, were produced from 140 samples obtained after a swab of skin lesions. The positive smear rate for the acid-fast bacilli (AFB) was, respectively, 16.4% and 12.9% for Dugomier and Ziehl-Neelsen staining. The ulceration with less than 1 year of evolution have high AFB rates of 15.8% for Ziehl-Neelsen staining and 21.1% for Dugomier's. Microscopic examination of skin exudate in face of ulceration, clinically suspected to be a Buruli's ulcer is not the best tool for biological diagnosis, due to poor technical sensibility. Nevertheless, it remains a good first means of investigation in an endemoepidemic area.-Authors' English Summary
Paiva, A. M., Vanderwall, I). E., Blanchard, J. S., Kozarich, J. W., Williamson, J. M. and Kelly, T. M. Inhibitors of dihydrodipicolinate reductase, a key enzyme of the diaminopimelate pathway of Mycobacterium tuberculosis. Biochim. Biophys. Acta 1545(2001)67-77.
Tuberculosis (TB) remains a leading cause of infectious disease in the world today and therapies developed over the last 40 years are becoming increasingly ineffective against resistant strains of Mycobacterium tuberculosis. In an effort to explore new mechanisms for drug development, we have investigated the enzymes of the diaminopimelate biosynthetic pathway as potential targets. Specifically, dihydrodipicolinate reductase, the essential gene product of dapB, was screened for novel inhibitors. Inhibitors were identified both by a molecular modeling approach which utilized the available crystal structure of the enzyme with an inhibitor bound at the active site as well as by more conventional screening strategies. The resulting compounds contain a number of structural motifs and were all found to be competitive with respect to the DHDP substrate. The K-i values for the inhibitors range from 10 to 90 uM. The molecular modeling approach was very effective in identifying novel inhibitors of the enzyme. These compounds were obtained at a higher frequency based on the number of compounds analyzed than those inhibitors discovered via conventional screening. However, conventional screening proved beneficial in identifying compounds with greater structural diversity. Authors' Abstract
Petricevich, V. L. and Alves, R. C. B. Role of cytokines and nitric oxide in the induction of tuberculostatic macrophage functions. Mediators Inflam. 9(2000)261-269.
The aim of this study was to determine phenotypic differences when BCG invades macrophages. Bacilli prepared from the same BCG primary seed, but produced in different culture media, were analyzed with respect to the ability to stimulate macrophages and the susceptibility to treatment with cytokines and nitric oxide (NO). Tumor necrosis factor (TNF) activity was assayed by measuring its cytotoxic activity on L-929 cells, interleukin-6 (IL-6) and interferon-gamma (IFN-γ) were assayed by enzyme-linked immunosorbent assay (ELISA); whereas NO levels were detected by Griess colorimetric reactions in the culture supernatant of macrophages incubated with IFN-γ. TNF or NO and subsequently exposed to either BCG-I or BCG-S. We found that BCG-I and BCG-S bacilli showed different abilities to simulate peritoneal macrophages. Similar levels of IL-6 were detected in stimulated macrophages with lysate from two BCG samples. The highest levels of TNF and IFN-γ were observed in macrophages treated with BCG-S and BCG-I. respectively. The highest levels of NO were observed in cultures stimulated for 48 hr with BCG-S. We also found a different susceptibility of the bacilli to exogenous treatment with IFN-γ and TNF which were capable of killing 60% and 70% of both bacilli; whereas NO was capable of killing about 98% and 47% of BCG-I and BCG-S, respectively. The amount of bacilli proportionally decreased with IFN-γ and TNF, suggesting a cytokine-related cytotoxic effect. Moreover, NO also decreased the viable number of bacilli. Interestingly, NO levels of peritoneal macrophages were significantly increased after cytokine treatment. This indicates that the treatment of macrophages with cytokines markedly reduced bacilli number and presented effects on NO production. The results obtained here emphasize the importance of adequate stimulation for guaranteeing efficient killing of bacilli. In this particular case, the IFN-γ and TNF were involved in the activation of macrophage bactericidal activity.Authors' Abstract
Portaels, F., Chemlal, K., Elsen, P., Johnson, P. D., Hayman, J. A., Hibble, J., Kirkwood, R. and Meyers, W. M. Mycobacterium ulcerans in wild animals. Rev. Sei. Tech. 20(2001)252-264.
Mycobacterium ulcerans infection, or Buruli ulcer, is the third most frequent mycobacterial disease in humans, often causing serious deformities and disability. The disease is most closely associated with tropical wetlands, especially in west and central Africa. Most investigators believe that the etiological agent proliferates in mud beneath stagnant waters. Modes of transmission may involve direct contact with the contaminated environment, aerosols from water surfaces, and water-dwellin« fauna (e.g.. insects). Person-to-person transmission is rare. Trauma at the site of skin contamination by M. ulcerans appears to play an important role in initiating disease. Once introduced into the skin or subcutaneous tissue, M. ulcerans multiplies and produces a toxin that causes necrosis. However, the type of disease induced varies from a localized nodule or ulcer, to widespread ulcerative or nonulcerative disease and osteomyelitis. Although culture of M. ulcerans from a patient was first reported in 1948, attempts to culture the mycobacterium from many specimens of flora and fauna have been unsuccessful. Failure to cultivate this organism from nature may be attributable to inadequate sampling, conditions of transport, decontamination and culture of this fastidious heat-sensitive organism. and to a long generation time relative to that of other environmental mycobacteria. Nevertheless, recent molecular studies using specific primers have revealed M. ulcerans in water, mud, fish and insects. Although no natural reservoir has been found, the possibility that M. ulcerans may colonize microfauna such as free-living amoebae has not been investigated. The host rage of experimental infection by M. ulcerans includes lizards, amphibians, chick embryos, possums, armadillos, rats, mice and cattle. Natural infections have been observed only in Australia, in koalas, ringtail possums and a captive alpaca. The lesions were clinically identical to those observed in humans. M. ulcerans infection is a rapidly re-emerging disease in some developing tropical countries. The re-emergence may be related to environmental and socioeconomic factors, for example, deforestation leading to increased flooding, and population expansion without improved agricultural techniques, thus putting more people at risk. Eradication of diseases related to these factors is difficult. Whether wild animals have a role in transmission is an important question that, to date, has been virtually unexplored. To address this question, surveys of wild animals are urgently required in those areas in which Buruli ulcer is endemic.-Authors' Abstract
Smith, D. A., Parish, T., Stoker, N. G. and Bancroft, G. J. Characterization of auxotrophic mutants of Mycobacterium tuberculosis and their potential as vaccine candidates. Infect. Immun. 69 (2001) 1142-1150.
Auxotrophic mutants of Mycobacterium tuberculosis have been proposed as new vaccine candidates. We have analyzed the virulence and vaccine potential of M. tuberculosis strains containing defined mutations in genes involved in methionine (metB), proline (proC), or tryptophan (trpD) amino acid biosynthesis. The metB mutant was a prototrophic strain; whereas the proC and trpD mutants were auxotrophic for proline and tryptophan, respectively. Following infection of murine bone marrow-derived macrophages, H37Rv and the metB mutant strain survived intracellularly for over 10 days; whereas over 90% of proC and trpD mutants were killed during this time. In SCID mice, both H37Rv and the metB mutant were highly virulent, with mouse median survival times (MST) of 28.5 and 42 days, respectively. The proC mutant was significantly attenuated (MST, 130 days); where as the trpD mutant was essentially avirulent in an immunocompromised host. Following infection of immunocompetent DBA mice with H37Rv, mice survived for a median of 83.5 days and the metB mutant now showed a clear reduction in virulence, with 2 of 5 infected mice surviving for 360 days. Both proC and trpD mutants were avirulent (MST of >360 days). In vaccination studies, prior infection with either the proC or trpD mutant gave protection equivalent (proC mutant) to or better (trpD mutant) than BCG against challenge with M. tuberculosis H37Rv. In summary, proC and trpD genes are essential for the virulence of M. tuberculosis, and mutants with disruptions in either of these genes show strong potential as vaccine candidates.-Authors' Abstract
Stahl, C., Kubetzko, S., Kaps, I., Seeber, S., Engelhardt, H. and Niederweis, M. MspA provides the main hydophilic pathway through the cell wall of Mycobacterium smegmatis. Mol. Microbiol. 40(2001)451-464.
MspA is an extremely stable, oligomeric porin from Mycobacterium smegmatis that forms water-filled channels in vitro. Immunogold electron microscopy and an enzyme-linked immunosorbent assay demonstrated that MspA is localized in the cell wall. An mspA deletion mutant did not synthesize detectable amounts of mspA mRNA, as revealed by amplification using mspA-specific primers and reversetranscribed RNA. Detergent extracts of the DeltamspA mutant exhibited a significantly lower porin activity in lipid bilayer experiments and contained about fourfold less porin than extracts of wild-type M. smegmatis. The chromosome of M. smegmatis encodes three proteins very similar to MspA. Sequence analysis of the purified porin revealed that mspB or mspC or both genes are expressed in the DeltamspA mutant. The properties of this porin, such as single channel conductance, extreme stability against denaturation, molecular mass and composition of 20-kDa subunits, are identical to those of MspA. Deletion of mspA reduced the cell wall permeability toward cephaloridine and glucose nineand fourfold, respectively. These results show that MspA is the main general diffusion pathway for hydrophilic molecules in M. smegmatis and was only partially replaced by fewer porins in the cell wall of the DeltamspA mutant. The minimal permeability coefficient of the DeltamspA mutant for glucose was 7.2 x 10s cm s_1, which is the lowest value reported so far for bacteria. This is the first experimental evidence that porins are the major determinants of the exceptionally low permeability of mycobacteria to hydrophilic molecules.-Authors' Abstract
Stockel, S., Meurer, M. and Wozel, G. Dapsone-induced photodermatitis in a patient with linear IgA dermatosis. Eur. J. Dermatol. 11(2001)50-53.
Dapsone (4, 4' diaminodiphenylsulfone) is an efficient antiinflammatory agent. Its therapeutic use may result in a variety of adverse effects. The most frequent unwanted reactions are hemolytic anemia and methemoglobinemia. By oral route dapsone is mainly metabolized to monoacetyldapsone (MADDS) and hydroxylamine dapsone (DDS-NOH). We report a 76-yearold female patient with linear IgA dermatosis who developed a dapsone-induced photosensitivity 8 weeks after initiation of sulfone therapy. She showed a widespread erythematous eruption in UV-exposed skin area. After clearing of skin lesions the photopatch test revealed positive reactions to dapsone, MADDS and DDS-NOH. Dapsone-induced photosensitivity to date has been described only in leprosy patients. We demonstrate for the first time that this adverse reaction is not restricted to leprosy and that dapsone metabolites may also contribute to the mechanism of photosensitivity like the parent sulfone. Dapsone-induced photosensitivity is a rare, not dose-related adverse effect of the sulfone and can also occur in patients with inflammatory skin disorders.-Authors" Abstract
Teo, S., Evans, ML, Ehrhart, J., Brockman, M., Allen, D., Morgan, M., Stirling, I), and Thomas, S. Lack of peripheral neuropathy in beagle dogs after 53 weeks oral administration of thalidomide capsules. Hum. Exp. Toxicol. 19(2000)615-622.
Thalidomide (Thalomid") is approved for use in the U.S. to treat complications from leprosy. Peripheral neuropathy is a doselimiting adverse event in humans. As part of a nonrodent regulatory toxicology study, Beagle dogs were fed orally via encapsulation for 53 weeks. A component of this study was to determine if the dogs developed peripheral neuropathy. Twenty-eight male and 28 female Beagle dogs approximately 8-10 months of age were used. They were dosed at 43, 200 or 1000 mg/kg for 53 weeks followed by a 4-week treatment-free recovery period. Nerve function was assessed by electrophysiological measurements of the tibial nerve prior to dosing and at weeks 13, 27, 38 and 5 I. Representative dogs from each group were sacrificed at 26, 53 and 58 weeks and histologic and ultrastructural evaluations were performed on the sural nerve. Thalidomide had no effect on sensory nerve conduction velocity, duration or amplitude of the action potential. At 27 weeks, mean sensory nerve action potential amplitude for females at 43 mg/kg was significantly greater than controls but was not evident at 39 weeks. Mean duration of sensory nerve action potential seemed to increase with similar magnitude over time in all dose groups including controls. Histological and ultrastructural evaluation of sections of sural nerve did not identify treatment-induced differences between control and thalidomide-dosed animals after 26 and 53 weeks of treatment. Additionally, no differences were observed following a 5-week treatment-free period at week 58. In contrast to humans, Beagle dogs did not develop thalidomide-induced peripheral neuropathy under conditions of the study.Authors' Abstract
Triccas, J. A., Britton, W. J. and Gicquel, B. Isolation of strong expression signals of Mycobacterium tuberculosis. Microbiology 147(2001)1253-1258.
The natural fluorescence of the Aequoria victoria green fluorescent protein was exploited to isolate strong expression signals of Mycobacterium tuberculosis. M. bovis bacillus Calmette-Guerin harboring M. tuberculosis fragments driving high levels of gfp expression were isolated by fluorescence-activated cell sorting (FACS). DNA sequencing and subsequent comparison with the M. tuberculosis genome sequence revealed that a total of nine postulated promoters had been identified. The majority of the promoters displayed activity that was greater than or equal to the M. fortuitum beta-lactamase promoter, one of the strongest mycobacterial promoters characterized to date. Two of the promoters corresponded to proteins predicted to be involved in calcium and magnesium utilization, the importance of such functions for cell physiology suggesting why these two genes are controlled by strong transcription signals. The seven other promoters corresponded to genes encoding proteins of unknown function. Promoter activity was maintained after prolonged incubation within macrophages, implying that these promoters could be used to drive sustained foreign gene expression in vivo. The strength of these expression signals identified could be employed for the overexpression of foreign genes in mycobacteria to aid protein purification and vaccine vector development. Furthermore, this study demonstrated that FACS provides a sensitive and efficient technique to measure and select strong mycobacterial expression signals.-Authors' Abstract
Valle, M. T., Megiovanni, A. M., Merlo, A., Pira, G. L., Bottone, L., Angelini, G., Bracci, L., Lozzi, L., Huygen, K. and Manca, F. Epitope focus, clonal composition and Th1 phenotype of the human CD4 response to the secretory mycobacterial antigen A«85. Clin. Exp. Immunol. 123(2001)226-232.
Lymphoproliferation of healthy donors was tested against mycobacterial antigens (PPD, Ag85, Ag85 peptides). All PPD responders recognized the secretory antigen Ag85 and the peptide specificity for Ag85B was defined. Peptide 91-108 was recognized by 85% of donors. In addition, all CD4 T-cell lines generated from 12 donors against PPD or Ag85 responded to 91-108. When this peptide was used to generate T-cell lines, the cells responded also to tuberculins from atypical mycobacterial species. Thus, the crossreactive peptide behaved as quasi-universal. The analysis of TCR-BV gene usage by cell lines showed that most Ag85-specific T cells correspond to the 91-108-specific clonotypes. Intracytoplasmic staining of cell lines after phorbol myristate acetate stimulation resulted in dominance of interferon-gamma (IFN-γ)IL-4 double-positive cells; whereas antigen stimulation resulted in production of IFN-γ only. The data show that peptide 91-108 is the major focus of the CD4 response to mycobacterial antigens in peripheral blood mononuclear cells and in T-cell lines from PPD responders.-Authors' Abstract
van Crevel, R., Vonk, A. G., Netea, M. G., Kullberg, B. J. and vander Meer, J. W. M. Modulation of LPS, PHAand M. tuberculosis-mtûvàied cytokine production by pentoxifylline and thalidomide. Eur. Cytokine Network 11(2000)574-579.
Pentoxifylline and thalidomide have been used to downregulate the production of TNF-alpha in several disease entities including mycobacterial infections and autoimmune disorders. These drugs inhibit the production of TNF-alpha by different mechanisms, but little is known about possible synergism and modulation of other cytokines. Pentoxifylline and thalidomide inhibited the in vitro stimulated production of TNF-alpha, IL-1 beta and IFN-gamma in blood mononuclear cells. No significant modulation of antiinflammatory cytokines was found. When used together, these agents demonstrated additive inhibition, but no synergism. Modulation of cytokine response was similar when different stimuli were used, including M. tuberculosis in tuberculin-positive individuals. Therefore, the balance between efficacy and toxicity may be more favorable when pentoxifylline and thalidomide are used together instead of either drug alone. Clinical studies are needed to establish this advantage when anticytokine strategies are considered.Authors' Abstract
Viveiros, M. and Aniaral, L. Enhancement of antibiotic activity against polydrug resistant Mycobacterium tuberculosis by phenothiazines. Int. J. Antimicrob. Agents 17(2001)225-228.
Phenothiazines have been shown to inhibit the in vitro growth of multidrugresistant (resistant to rifampin and isoniazid) Mycobacterium tuberculosis (MDRTB). They have been considered as potential adjuvants to regimens employing four or more antibiotics for the management of freshly diagnosed infections of M. tuberculosis in patients from areas known to have a high prevalence of MDRTB. Chlorpromazine has been shown to enh; ince the activity of antibiotics (except ethambutol) to which M. tuberculosis is susceptible. This might result in a reduction in the dose of some or all of the antibiotics employed without sacrificing the integrity of treatment. Chlorpromazine, thioridazine and promethazine were shown to enhance the activity of rifampin and streptomycin when used in combinations at concentrations that are minimally effective when employed separately against clinical strains of M. tuberculosis resistant to two or more antibiotics (poly-drug resistant MTB). the phenothiazines had no effect on the activity of isoniazid against poly-drug resistant MTB.-Authors' Abstract
Walsh, D. S., Prieto-Go, D., Abalos, R. M., Tuur-Saunders, S. M., Villahermosa, L. G., Jabien, Z., Walsh, G. P. and Fajardo, T. T. Malignant T-cell lymphoma mimicking lepromatous leprosy. Clin. Exp. Dermatol. 26 (2001)173-175.
We describe a 16-year-old Filipino boy who presented with skin lesions highly suggestive of lepromatous leprosy, but further assessment established a diagnosis of malignant T-cell lymphoma. This case emphasizes the extensive differential diagnosis of leprosy, as well as the importance of obtaining skin biopsies for diagnostic confirmation.-Authors' Abstract