- Volume 69 , Number 2
- Page: 119–22
Leprosy with peripheral T-Cell lymphoma: a rare association
To the Editor:
An 85-year-old male presented with otherwise asymptomatic skin lesions over the face of 8 months' duration. He did not have any other cutaneous or systemic complaints. He had undergone rectal surgery 15 years earlier, but details of the disease or the surgery were not available. Examination revealed numerous, firm-to-hard, skin- colored and erythematous papules and nodules predominantly over the face, giving rise to "leonine fades," with a few lesions also over the trunk (Fig. 1 ). One lesion over the face (Fig. 1 ) and another over the back were fungating. In addition, his skin showed diffuse leathery induration over the trunk and extremities. He was fairly well built and not anemic. The axillary lymph nodes were 2-3 cm in diameter, firm in consistency and were not fixed to the underlying structures. Systemic examination did not reveal any abnormalities. Peripheral nerves were not thickened. A hemogram and liver and renal function tests were normal. USG-abdomen showed fatty liver. No para-aortic nodes were seen. A slit-skin smear by the standard technique demonstrated acid-fast bacilli occurring both singly and as globi (Fig. 2) |bacterial index (BI) = 6+; morphological index (MI) = 1.7]. A skin biopsy from the nodular lesion over the back showed a thin epidermis, a clear grenz zone and focal collection of macrophages (Fig. 3) which were positive with Fite staining (Fig. 4). In addition, dense aggregates of atypical lymphocytes were seen in the upper dermis (Fig. 3) and also around the follicle; they were uniformly positive for the pan T marker (CD3), suggesting a clonal population.
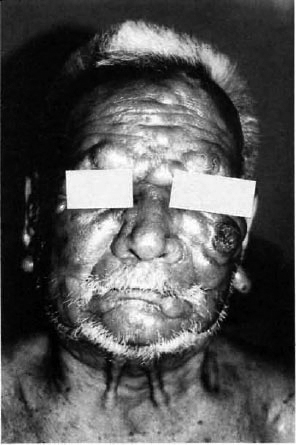
Fig. 1. Multiple papules and nodules over the face.
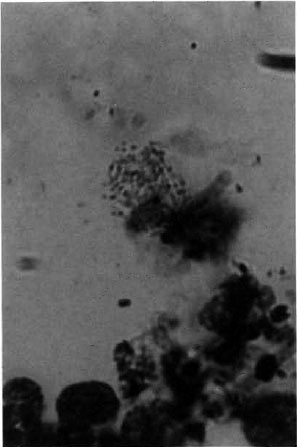
Fig. 2. Photomicrograph of slit-skin smear showing macroM. leprae (Ziehl-Neelsen x 1000).
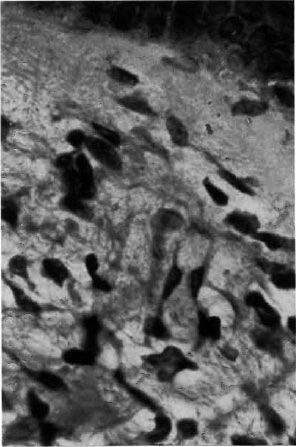
Fig. 3. Photomicrograph showing focal macrophage granuloma and collection of atypical lymphocytes in the upper dermis (H&E x 1000).
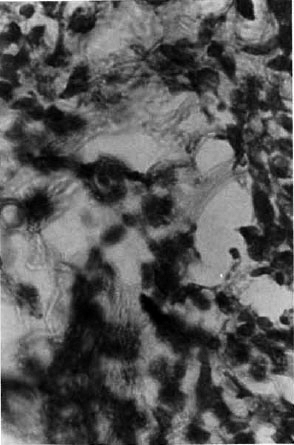
Fig. 4. Photomicrograph showing M. leprae inside macrophages (File x 1000).
A fine needle aspiration cytology (FNAC) smear from the left axillary lymph node showed a relatively uniform population of cells. The nuclei displayed aniso- karyosis with dense chromatin. Occasional nuclei showed indented nuclear outlines. Mitoses were frequently observed. No Reed-Sternberg cells were seen (Fig. 5). These cytological features were suggestive of lymphoma (non-Hodgkin's type). A lymph node biopsy was advised for confirmation and typing, but the patient refused the biopsy.
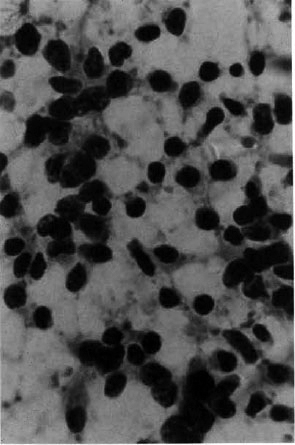
Fig. 5. Photomicrograph of FNAC lymph node indicating a uniform population of cells showing anisokaryosis, nuclear convolution and mitoses (Giemsa x 1000).
The association of leprosy with various visceral and lymphoreticular malignancies is known (2). In a series of 252 autopsies done in leprosy patients, the incidence of malignant tumor was 33.7% (85 cases) and carcinoma of the gastrointestinal tract was the most common tumor followed by carcinoma of the lung, the incidence of which has increased in recent years (2). Of the nonepithelial malignancies, malignant lymphoma is the most common association and these incude Hodgkin's lymphoma and mycoses fungoides (2, 3, 5, 6). The present case had the classical "leonine facies" of lepro- matous (LL) leprosy but the nodules over the face were unusually firm-to-hard in consistency and a few nodules were fungating. These features raised the suspicion of an underlying malignancy, and the skin biopsy showed a dense collection of CD3+ (pan T marker) atypical lymphocytes in the dermis along with focal macrophage granuloma which was positive by Fite staining. There was no epidermotrophism, the feature of mycosis fungoides. Multiple cutaneous nodules without any patch or plaque and the absence of epidermotrophism in the present case are features that favor peripheral T-cell lymphoma (PTL), otherwise known as pleomorphic, small/medium size, cutaneous T-cell lymphoma (1). Clinically, most of the patients with PTL present with Iymph- adenopathy. Skin and/or mucosal involvement is seen in 50% of the patients. The risk of peripheral blood involvement is seen in 30% of the patients, and is closely associated with cutaneous involvement (4). The T-cell immunophenotype is that of CD4+ cells, often with the loss of pan T-cell antigens (1). Clonal rearrangement of the T-cell receptor gene is often detected (1).
The occurrence of double or triple cancers in leprosy has also been reported (2). It is not very clear whether leprosy patients are at risk for development of neoplasia or patients with neoplasms are more prone to develop leprosy. Another interesting feature in this case is the absence of clinically evident nerve thickening. Clinically pronounced skin involvement is known to occur before nerve thickening in LL patients compared to patients at the tuberculoid pole of the leprosy spectrum. It is also possible that the malignancy is responsible for the rapid progression of skin lesions in LL patients.
- Gomathy Sethuraman, M.D.
Serisha, D.V.D.
Chakravarthi Rangachari Srinivas, M.D.
Professor and Head
Department of Dermatology
PSG Hospitals
Coimbatore 641004
Tamil Nadu, India.
- Sonaimuthupillai Byravarathinam, M.D.
Rtd. Professor and Head
Department of Dermatology
Coimbatore Medical College
Coimbatore, India.
- Manjeri Lakshmanan Raman, M.D.
Consultant Pathologist
GKNM Hospital
Coimbatore, India.
- Leslie Smiles, M.D.
Subba Rao, M.D.
Department of Pathology
PSG Hospitals
Coimbatore, India.
REFERENCES
1. Duncan, L. M. Cutaneous lymphoma: understanding the few classification schemes. Dermatol. Clin. 17(1999) 569-592.
2. Furuta, M, Obara, A.. Ishida, Y., Harada, N. and Ozaki, M. Leprosy and malignancy: autopsy findings of 252 leprosy patients. Int. J. Lepr. 58 (1990)697-702.
3. Grossman, D., Rapini, R. P., Osborne, B. and Du- vic, M. Emergence of leprosy in a patient with mycosis fungoides J. Am. Acad. Dermatol. 30 (1994)313-315.
4. Jaffe, E. S. Post-thymic T cell lymphomas. In: Surgical Pathology of the Lymph Nodes and Related Organs. 2nd edn. Jaffe, E. S., ed. Philadelphia: W. B. Saunders Company, 1995, pp. 344-389.
5. Levy, M. L.. Rosen. T., Tschen, J. A.. McGavran, M. H. and Kalter, D. C. Hansen's disease following lymphoma. J. Am. Acad. Dermatol. 15 (1986) 204-208.
6. Weshler, Z., Leviatan, A., Gordon, R. and Kopolovic, J. Development of Hodgkin's disease in a patient with leprosy. J. Oncol. 35 (1978) 281-284.
Reprint requests to Dr. C. R. Srinivas at the above address or fax 91-422-594400; e-mail: psgimsr@md3.vsnl.net.in