- Volume 65 , Number 1
- Page: 101–2
"Umbilicated" lesions in histoid leprosy
To the Editor:
Histoid leprosy is a well-recognized entity, the exact pathogenesis of which is still elusive (2). It is essentially characterized by cutaneous and/or subcutaneous nodules and plaques present over apparently normal skin with unique histopathology and a characteristic bacterial morphology.
Case report. A 37-year-old male patient presented with multiple, firm, skin-colored nodules with very well-defined edges, predominantly involving the lower back (Fig. 1), buttocks and abdominal skin (Fig. 2) with a few lesions also over the chest and lower part of the face. A distinctly umbilicated nodule was present over the lower back (henceforth referred to as lesion 1 in Fig. 1) and a cluster of lesions showing a tendency toward coalescence, giving a pseudoumbilicated appearance (henceforth referred to as lesion 2 in Fig. 1) can be seen a little above lesion 1 (Fig. 1). The patient was asymptomatic apart from the nodular lesions. There was no history of any skin disease in the family, and the patient had not been treated earlier for any skin ailment.
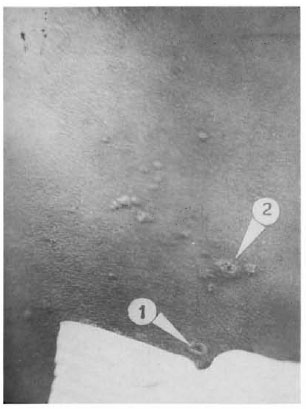
Fig 1. Nodular histoid lesions over the hack showing "umbilicated- lesions ( 1 and 2).
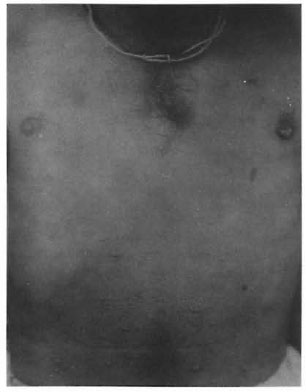
Fig . 2. Nodular histoid lesions over the anterior abdominal skin.
A general physical examination and laboratory studies, including a complete blood cell count, chemistry screen, urinalysis, erythrocyte sedimentation rate and liver function studies, showed no abnormalities. An ophthalmological examination also showed no abnormalities and no neural functional deficit could be elicited. Skin-slit smears taken by the standard method from these lesions revealed an abundance of acid-fast bacilli (AFB) occurring singly, in clusters and as globi. Histological study of excisional biopsies of these lesions showed the characteristic circumscribed histoid lepromas characterized by the predominance of spindle-shaped cells and an abundance of long AFB (compared to ordinary lepra bacilli) confirming the clinical diagnosis of histoid leproma.
The patient was put on standard World Health Organization multiple drug therapy (WHO/MDT) composed of dapsone, rifampin and clofazimine. An extremely favorable response to this WHO/MDT was obtained after 2 ½ years of therapy, with the lesions becoming inactive clinically as well as histologically. The patient was released from treatment at this time. The patient did not experience any kind of reactional episodes during the treatment or after stopping the treatment, until the date of submission of this report.
Discussion. Ramanujam and Ramu (1), in their masterly treatise on histoid leprosy, stated that the cutaneous histoids lack umbilication, so typical of molluscum contagiosum, but Singh, et al. described a case of histoid leprosy in which most of the lesions were umbilicated (3). In the case which I have reported here, while an umbilicated lesion is distinctly visible (lesion I), lesion 2 seems to give the appearance of umbilication due to the coalescence of the nodular lesions arranged closely in a ring-like fashion. A very favorable response to WHO/ MDT observed in this case lends credence to the view that histoid leprosy is not the offshoot of sulfone resistance for the simple reason that the patient had never taken sulfone treatment before.
The author has published this case to stress that while true umbilication may be occurring in some lesions of a histoid leproma, in the other "umbilicated" lesions it may not be a true process, and that the prognosis of histoid leproma is not decidedly unfavorable.
- Ashok K. Sharma, M.D.
Mahatma Gandhi Institute of Medical Sciences
Department of Dermatology
Sewagram
Wardha, M.S., India
REFERENCES
1. RAMANUJAM, K. and RAMU, G. Wade's histoid lepromatous leprosy. Lepr. India 41(1969)347-351.
2. SEHGAL, V. N. and SKIVASTAVA, G. Histoid Leprosy. Delhi: CBS Publishers and Distributors, 1985, p. 1.
3. SINGH, M., KANWAR, A. J. and MALHOTRA, Y. K. An unusual presentation of histoid leprosy. GaryounisMed. J. 4(1981)91-92.
Reprint requests to: Dr. Ashok K. Sharma, Assistant Professor. Department of Skin & STD. I. G. Medical College, Shimla, H.P., India.